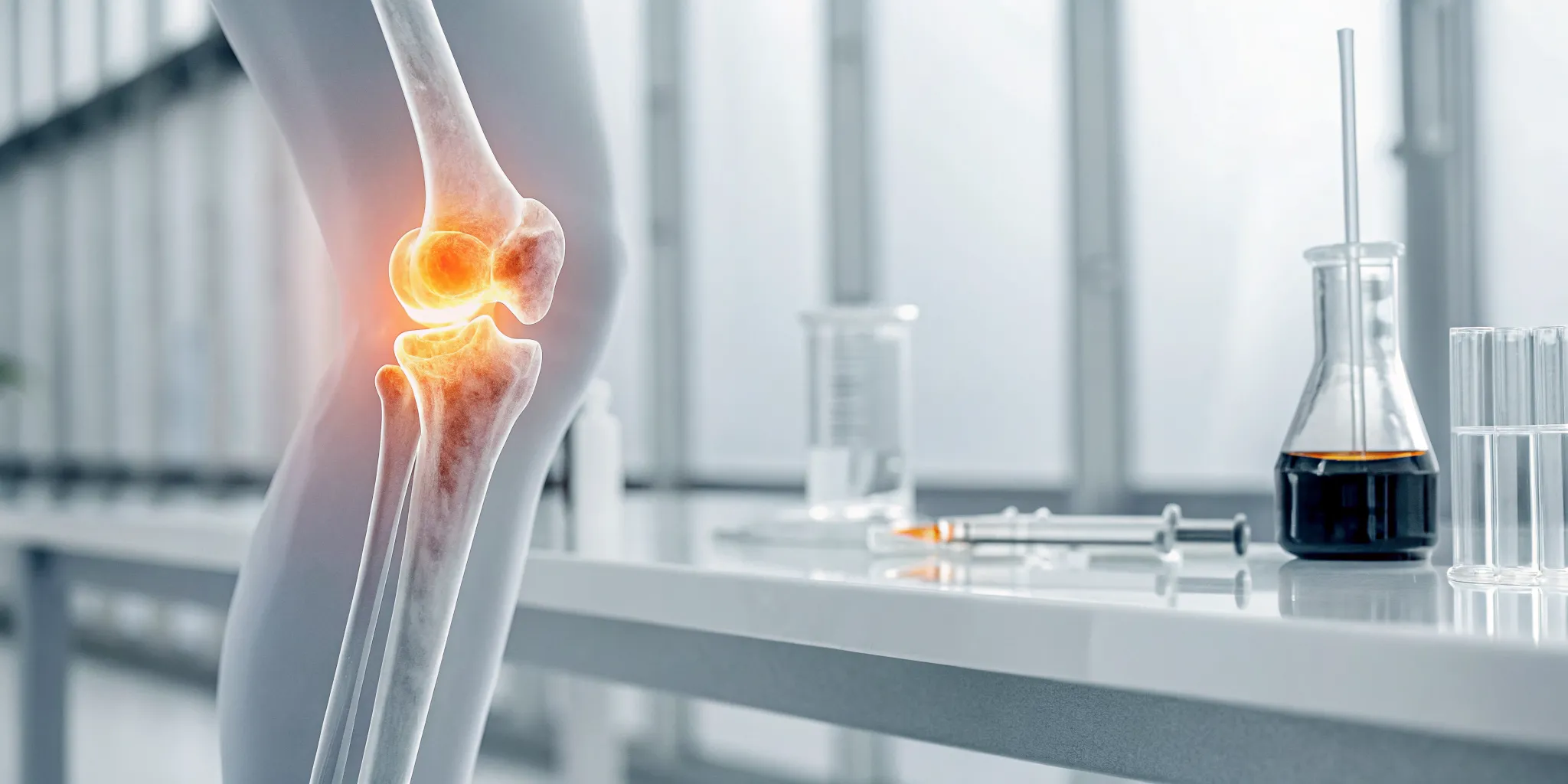
Think of regenerative medicine as a specialized toolkit for repairing your body. Two of the most effective tools for joint pain are PRP and stem cell therapy. PRP acts like a powerful foreman, sending signals that call your body’s own repair crews to the site of an injury. Stem cells, on the other hand, are the master builders, capable of creating brand new tissue to replace what’s been lost. The question of PRP vs stem cell for joint pain is really about choosing the right tool for the job. This guide will explain what each tool does best, helping you understand which approach is better suited for your specific repair project.
Key Takeaways
- PRP supports healing while stem cells rebuild tissue: PRP uses concentrated growth factors from your own blood to signal and accelerate your body’s natural repair process. Stem cell therapy is different; it introduces new cells that can actively regenerate lost or damaged tissue, like cartilage.
- Your diagnosis determines the right treatment path: For milder conditions like early arthritis or tendon injuries, PRP can provide an effective healing boost. For more advanced joint degeneration or significant cartilage damage, stem cell therapy is often the more powerful option for lasting repair.
- A professional consultation is your essential first step: Regenerative medicine is highly personalized, not a one-size-fits-all solution. A thorough evaluation with a specialist is the only way to create a safe, effective treatment plan based on your specific condition and health goals.
PRP vs. Stem Cell Therapy: What Are They?
When you’re exploring options for joint pain, you’ll likely come across two powerful regenerative treatments: PRP and stem cell therapy. While both are designed to help your body heal itself and avoid surgery, they work in very different ways. Understanding the fundamentals of each treatment is the first step in figuring out which path might be right for you. Let’s look at what each one is and how it helps your body recover.
How PRP Therapy Works
Think of PRP, or Platelet-Rich Plasma, as a concentrated dose of your body’s own healing power. The process starts by drawing a small amount of your blood, similar to a routine lab test. This blood is then placed in a centrifuge, a machine that spins it at high speed to separate the components. This spinning process isolates and concentrates the platelets, creating a golden, platelet-rich plasma. This plasma is full of growth factors, which are proteins that signal your cells to repair damage and reduce inflammation. The resulting PRP therapy is then injected directly into your injured joint, giving your natural healing process a major assist.
How Stem Cell Therapy Works
Stem cell therapy takes a different approach by introducing new, versatile cells to the site of your injury. Stem cells are essentially the body’s “blank slate” cells. They have the remarkable ability to develop into many different types of specialized cells, such as cartilage, bone, or muscle tissue. At Miami Stem Cell, we use umbilical cord-derived mesenchymal stem cells (MSCs), which are ethically sourced and highly potent. When these powerful stem cells are injected into a damaged joint, they can replace worn-out cells and actively regenerate new, healthy tissue, addressing the root cause of the degeneration and pain.
How They Relieve Pain and Promote Healing
Both treatments aim to relieve pain and promote healing, but they are best suited for different situations. PRP is excellent for speeding up the recovery of tissues that are slow to heal, like tendons and ligaments. It reduces swelling and pain by enhancing your body’s existing repair mechanisms. It’s like sending in reinforcements for your body’s own construction crew. On the other hand, stem cell therapy is often the better choice when tissue is significantly damaged or lost, as seen in conditions like osteoarthritis where cartilage has worn away. Stem cells don’t just support the healing process; they actively rebuild what’s been lost. This makes them a powerful tool for joint regeneration and addressing more advanced degenerative conditions.
How Do PRP and Stem Cell Treatments Differ?
While both PRP and stem cell therapy fall under the umbrella of regenerative medicine, they work in fundamentally different ways. Think of them as two unique tools designed for different jobs. The main distinctions come down to what they are made of, how they are prepared, and the specific way they help your body heal. Understanding these differences is the first step in figuring out which approach might be the right fit for your joint pain and long-term health goals. Let’s break down what sets them apart.
Source and Preparation Methods
The first major difference is where the therapeutic agents come from. PRP therapy uses your own blood. The process is straightforward: we draw a small amount of your blood and place it in a centrifuge. This machine spins the blood at high speeds to separate the platelets and plasma from other blood cells, creating a concentrated platelet-rich plasma that is ready for injection.
Stem cell therapy, on the other hand, uses powerful, undifferentiated cells that can develop into many different cell types. At Miami Stem Cell, we use ethically sourced, umbilical cord-derived mesenchymal stem cells (MSCs). These cells are collected from the umbilical cords of healthy, full-term births and processed in a specialized lab, ensuring a high concentration of potent, young cells without an invasive procedure for you.
Comparing the Treatment Procedures
Because PRP is created from your own blood, the entire procedure is typically completed in a single visit. The blood draw, preparation, and injection usually take about an hour. It’s a relatively quick and simple process that gets you in and out of the office efficiently.
The procedure for stem cell therapy is also a simple injection, but the preparation of the cells is far more complex. Since we use carefully screened and processed umbilical cord-derived stem cells, the collection and lab preparation happen long before your appointment. For you, the patient, the process is just as simple as a PRP injection. This approach allows you to receive a high dose of powerful, viable cells without undergoing an invasive harvesting procedure, like a bone marrow aspiration, which is required when using your own stem cells.
Comparing Their Regenerative Abilities
This is where the two treatments really diverge. PRP acts as a powerful signaling agent. The concentrated growth factors in the platelets send messages to your body, calling your own repair cells to the injured area and reducing inflammation. It essentially gives your natural healing process a major push.
Stem cells, however, are the actual builders. They do more than just send signals; they can directly replace damaged cells and regenerate new tissue. For conditions where tissue has been lost or severely degraded, like in advanced arthritis or significant cartilage damage, stem cells offer a unique ability to rebuild what has been worn away. They are foundational to creating new, healthy tissue, not just repairing what’s already there.
Weighing the Benefits and Risks of Each Treatment
Deciding between PRP and stem cell therapy involves looking at your specific injury, your long-term goals, and what each treatment can realistically offer. Both are promising non-surgical options, but they work differently and come with their own set of considerations. Think of PRP as a powerful supporter for your body’s existing repair crew, while stem cell therapy is like calling in specialized reinforcements to rebuild. Understanding the unique advantages and potential downsides of each is the first step toward making an informed choice for your joint health.
The Pros and Safety of PRP Therapy
One of the biggest advantages of PRP therapy is its excellent safety profile. Because the treatment uses a concentrate of your own blood, the risk of an allergic reaction or your body rejecting the treatment is virtually zero. It’s a very natural approach that gives your body’s healing mechanisms a helping hand, rather than introducing a foreign substance. PRP is great for encouraging the cells you already have to work more efficiently. It’s also generally more affordable and less invasive than other regenerative options, making it an accessible starting point for many people dealing with mild to moderate joint pain or soft tissue injuries.
The Pros and Limitations of Stem Cell Therapy
Stem cell therapy takes a more direct approach to healing. Unlike PRP, which supports existing cells, stem cells have the unique ability to develop into new, specialized cells. This means they can potentially replace tissue that has been damaged by injury or degenerative conditions like arthritis. This makes stem cell treatments a powerful option for more advanced joint issues where tissue has been lost. The main limitations are that the procedure is more complex and represents a greater financial investment. However, for those with significant cartilage damage or chronic conditions, the potential for true tissue regeneration is a major benefit that can lead to lasting relief.
Side Effects and Recovery: What to Expect
For both PRP and stem cell injections, the recovery process is fairly straightforward. You can expect some temporary soreness, swelling, or inflammation at the injection site as your body’s healing response kicks in. This is a normal and even positive sign that the treatment is working. Your doctor will give you specific instructions, which usually include resting the joint and avoiding strenuous activity for a short period, often one to two weeks. It’s important to follow these guidelines to give the platelets or stem cells the best possible environment to do their job. You can find answers to more specific questions about recovery on our FAQs page.
Which Joint Conditions Respond Best to Each Therapy?
Deciding between PRP and stem cell therapy isn’t about which one is universally “better,” but which one is better for you. The right choice depends entirely on your specific diagnosis, the severity of your joint damage, and your long-term wellness goals. Think of it this way: PRP is excellent at stimulating and amplifying your body’s existing healing processes, while stem cell therapy focuses on regenerating and replacing tissues that are too damaged to repair on their own.
Both treatments offer a path toward relief and recovery without invasive surgery, but they work on different scales. For milder issues or injuries that just need a helping hand to heal properly, PRP can be a powerful tool. For more chronic conditions, advanced degeneration, or significant tissue loss where the body’s own repair mechanisms are overwhelmed, stem cell therapy often becomes the more appropriate and effective option. Understanding how each therapy matches up with specific joint conditions is the first step toward making an informed decision with your doctor.
Osteoarthritis and Cartilage Damage
For those dealing with the daily aches of mild to moderate osteoarthritis, PRP therapy is often a great starting point. It can help reduce the pain and stiffness that limit your activities and improve overall joint function. Because PRP uses your own blood’s growth factors, it gives your body a concentrated signal to address inflammation and support cartilage health. However, when osteoarthritis is more advanced or there is significant cartilage loss, the focus may shift to joint regeneration. This is where stem cell therapy shines, as it introduces new cells that have the potential to repair and replace damaged cartilage, addressing the root cause of the degeneration rather than just managing symptoms.
Sports Injuries and Soft Tissue Trauma
If you’ve experienced an acute injury like a tendon strain, ligament sprain, or muscle tear, PRP can be incredibly effective. It’s particularly good for injuries that are slow to heal on their own, giving the damaged tissue the concentrated dose of growth factors it needs to kickstart a more robust recovery. For more severe trauma, such as a complete ligament tear or a chronic tendon issue that hasn’t responded to other treatments, stem cell therapy may be recommended. Stem cells are often used when tissues are badly damaged because they can help rebuild the structure of the injured area, offering a more comprehensive approach to pain management and healing.
Advanced Joint Degeneration
When joint damage is severe and chronic, stem cell therapy is typically the more powerful solution. In cases of advanced osteoarthritis where cartilage has significantly worn away, the joint needs more than just a signal to heal; it needs new material to rebuild. Stem cells are uniquely suited for this task, as they can differentiate into the specific cell types needed to repair the joint. While PRP can still offer some anti-inflammatory benefits, most studies show that stem cell-based therapies provide more effective and lasting pain relief for these more serious conditions, making it the preferred choice for significant joint degeneration.
What to Expect During Treatment and Recovery
Deciding on a regenerative treatment is a big step, and it’s natural to wonder what the process actually looks like. Knowing what happens before, during, and after your procedure can help you feel more confident and prepared. Both PRP and stem cell therapies are minimally invasive, in-office procedures designed to get you back to your life with minimal downtime. The goal is to work with your body’s natural healing mechanisms to repair joint damage from the inside out. Let’s walk through what you can expect from preparation to recovery.
Preparing for Your PRP Injection
The process for PRP therapy is quite straightforward and uses your body’s own healing components. It all starts with a simple blood draw, similar to what you’d have done for a routine lab test. We take a small sample of your blood and place it in a centrifuge, a machine that spins at high speed to separate the different elements. This process concentrates the platelets and growth factors into a powerful solution called platelet-rich plasma. Once this golden liquid is ready, your doctor carefully injects it directly into the injured joint, delivering a potent healing boost right where you need it most.
The Stem Cell Therapy Process
Our approach to stem cell therapy harnesses some of the most powerful healing cells available. We use ethically sourced, umbilical cord-derived mesenchymal stem cells (MSCs). These cells are special because they have the remarkable ability to develop into the specific types of cells your body needs for repair, like cartilage, ligament, or tendon cells. The procedure itself is simple: your doctor injects these prepared stem cells into the damaged joint. This targeted delivery helps kickstart your body’s repair process, encouraging the growth of new, healthy tissue and addressing the root cause of your joint pain.
Your Recovery and Follow-Up Care
After either a PRP or stem cell injection, your body gets to work on the healing process. You might experience some mild soreness or swelling at the injection site, which is a normal sign that the regenerative cascade has begun. Your doctor will provide specific aftercare instructions, which usually involve a short period of rest followed by a gradual return to normal activity. Following this guidance is key to achieving the best possible outcome. Many patients undergoing joint regeneration start to notice significant improvements within a few weeks to a month as the new tissue develops and inflammation subsides. We’ll schedule follow-up appointments to monitor your progress and ensure your recovery is on track.
How Do Costs and Insurance Coverage Compare?
When you’re considering regenerative treatments, the financial aspect is naturally a big part of the conversation. Both PRP and stem cell therapy are investments in your long-term joint health and quality of life. Understanding the costs involved, and what to expect from insurance, helps you make a clear and confident decision. Let’s break down what goes into the cost of each treatment so you can plan accordingly.
Understanding the Cost of PRP
Generally, PRP therapy is the more accessible option from a cost perspective. The final price isn’t just for the injection; it covers the entire process, including your initial consultation, the blood draw, processing your platelets, and any necessary follow-up appointments. The total cost can vary depending on the joint being treated and how many sessions you might need to achieve your desired results. Because it uses your own blood, the procedure is less complex than stem cell therapy, which is reflected in the price. It’s a powerful, focused treatment that offers a great starting point for many people dealing with joint pain.
The Investment in Stem Cell Therapy
Stem cell therapy represents a more significant investment, and for good reason. The procedure is more intricate, involving highly specialized lab processes to prepare the cells for treatment. At Miami Stem Cell, we use potent mesenchymal stem cells (MSCs) sourced from umbilical cord tissue, which offers a powerful regenerative capacity. This advanced approach to joint regeneration addresses damage at the cellular level, aiming for more comprehensive and lasting repair. Think of it less as a simple cost and more as a long-term investment in restoring function and avoiding more invasive procedures, like surgery, down the road.
Understanding Insurance and Payment Options
It’s important to know that most insurance plans do not cover PRP or stem cell therapies. Because these treatments are still considered elective by many insurance carriers, you should plan for them to be an out-of-pocket expense. The best first step is to get a clear and personalized cost estimate based on your specific condition and treatment plan. We believe in full transparency, so we encourage you to contact our clinic for a detailed breakdown. We can also discuss flexible financing options to help make these transformative treatments more accessible for our patients.
The Science: What Does Research Say About Effectiveness?
When you’re exploring treatments for joint pain, you want to know what works. Both PRP and stem cell therapy are backed by a growing body of scientific research, but it’s helpful to understand what the studies actually say. The field of regenerative medicine is constantly evolving, with new findings helping doctors refine treatment protocols and improve patient outcomes. While many studies show promising results, it’s also important to recognize that outcomes can vary, and research is still ongoing to determine the best applications for each therapy.
Looking at the evidence helps you set realistic expectations and have a more informed conversation with your doctor. The goal is to find a treatment that not only addresses your pain but also supports your body’s ability to heal itself. At Miami Stem Cell, we focus on science-backed therapies that are tailored to your specific condition, ensuring your treatment plan is built on a solid foundation of clinical research. Let’s look at what the current science says about PRP and stem cell therapy for joint pain.
What Studies Show About PRP
Research on PRP therapy often highlights its effectiveness in reducing pain and improving function, especially for conditions like knee osteoarthritis. For example, a 2022 double-blind study from the NIH found that while both PRP and cortisone were effective, PRP showed a more significant and lasting reduction in pain over time. This suggests that PRP may offer more durable relief than traditional injections.
Another review of injection therapy in knee osteoarthritis found that a single PRP injection could reduce joint pain more effectively and for a longer period than other options. The research indicates that PRP not only alleviates symptoms but also enhances overall quality of life for patients dealing with chronic joint issues. These studies support the use of PRP therapy as a reliable, non-surgical option for managing joint pain.
What Studies Show About Stem Cell Therapy
Stem cell therapy is one of the most exciting areas of regenerative medicine, with research pointing to its powerful healing potential. A large meta-analysis of 18 studies concluded that mesenchymal stem cell (MSC) injections were effective for knee pain for up to two years, significantly improving both pain levels and joint function. This is the type of therapy we specialize in, using potent umbilical cord-derived stem cells.
While the results are promising, it’s important to note that research is ongoing. Some smaller studies have reported mixed results, showing short-term pain improvement but calling for more data on long-term effectiveness. This variability underscores why a personalized approach is so critical. By evaluating your specific case of joint degeneration, we can determine if you are a good candidate for this advanced treatment.
A Look at Long-Term Success
When considering long-term results, the scientific community is still gathering data. Some studies suggest that the effectiveness of regenerative treatments can depend on the specific condition and the individual patient. For instance, one stem cell therapy study found that over the course of a year, cell therapy was not universally superior to corticosteroids for pain relief, highlighting that it may not be the best fit for everyone.
However, other research points to the significant advantages of cellular treatments. A review of advancements in regenerative therapies found that stem cell-based therapies provided the most effective pain relief when compared to other options. This evolving landscape of research shows why it’s so important to work with a provider who understands the science and can create a personalized plan for your long-term joint health.
Common Myths About Regenerative Joint Treatments
When you’re exploring new treatments for joint pain, it’s easy to run into conflicting information. Regenerative medicine is an exciting field, but it’s also filled with myths and exaggerated claims that can be confusing. Getting clear on the facts is the first step toward making a confident decision about your health. Let’s walk through some of the most common misunderstandings so you can separate fact from fiction.
Being an informed patient is your greatest asset. Understanding what to realistically expect from treatment, the importance of regulatory standards, and how to spot a trustworthy provider will help you find a safe and effective path forward. We’ll break down what you need to know about treatment timelines, FDA guidelines, and evaluating the claims you might encounter online or in clinics. This knowledge empowers you to ask the right questions and choose a treatment plan that truly aligns with your health goals.
Setting Realistic Timelines for Results
One of the biggest myths is that regenerative treatments offer instant pain relief. While some people might feel better shortly after a procedure, these therapies are not a quick fix. Unlike a steroid shot that masks pain, regenerative medicine works by signaling your body to repair itself. This is a biological process that takes time. True healing happens on a cellular level as tissues are gradually repaired and inflammation subsides.
Think of it as planting a garden. You don’t see a full bloom overnight. It takes weeks and sometimes months for the seeds to sprout and grow strong. Similarly, you should expect to see gradual improvements in the weeks and months following your treatment. Your care team will outline a specific timeline for you, but patience is a key part of the process as your body does the restorative work.
Understanding FDA Regulations
The regulatory landscape for stem cell therapy can be tricky, and it’s crucial to understand it for your safety. A common misconception is that all stem cell treatments offered in the U.S. are FDA-approved. In reality, the FDA has very strict guidelines. Many clinics use cells sourced from the patient’s own fat or bone marrow, which are manipulated in ways that may not meet FDA standards for safety and efficacy.
At Miami Stem Cell, we exclusively use umbilical cord-derived mesenchymal stem cells (MSCs) sourced from accredited tissue banks. This approach adheres to the FDA’s rigorous regulations for cellular products. Understanding the difference between overseas vs. USA stem cell treatments and the importance of regulatory compliance is essential for ensuring you receive a safe and high-quality therapy. Always ask a provider about their cell source and their adherence to FDA guidelines.
Evaluating Provider Claims and Safety
With the growing interest in regenerative medicine, many clinics have appeared, some making bold promises that aren’t backed by science. Be cautious of anyone guaranteeing a cure or promoting a one-size-fits-all approach. Effective regenerative therapy is highly personalized. Your treatment plan should be based on a thorough evaluation of your specific joint condition, overall health, and long-term goals.
A reputable provider will be transparent about what the therapy can and cannot do. They will base their recommendations on clinical evidence and be open to answering all your questions. Don’t hesitate to ask about their experience, the specifics of their protocols, and the scientific research supporting their methods. A provider who is committed to your well-being will welcome your questions and provide clear, honest answers. You can learn more about our science-backed approach and our commitment to patient education.
How to Choose the Right Treatment for Your Joint Pain
Deciding between PRP and stem cell therapy isn’t about picking the “best” option, but the best option for you. Your body, your injury, and your long-term goals are unique, and your treatment plan should be too. Making an informed choice starts with understanding how your specific situation aligns with what each therapy offers. By looking closely at your condition, your overall health, and asking the right questions, you can work with your doctor to find the most effective path toward healing and getting back to the life you love.
Assess Your Condition and Goals
The first step is to get a clear picture of what’s happening inside your joint. The nature and severity of your condition play the biggest role in this decision. PRP therapy is often a great starting point for mild to moderate issues, like early-stage arthritis or tendonitis, where the body just needs a concentrated push to accelerate its natural healing process. However, if you’re dealing with more advanced joint degeneration or significant cartilage loss, stem cell therapy may be the more appropriate choice. It’s designed for situations where tissues need to be fundamentally repaired and regenerated, not just encouraged to heal.
Consider Your Overall Health and Lifestyle
Your general health and daily activities also factor into the equation. Because PRP therapy uses a concentration of platelets from your own blood, it’s an incredibly safe procedure with minimal risk of adverse reactions. It’s an excellent way to harness your body’s inherent healing abilities. On the other hand, stem cell therapy introduces powerful, new cells that have a robust capacity to differentiate and rebuild damaged tissue, making it a more potent regenerative option. Think about your lifestyle, too. An active athlete aiming for peak performance might have different needs than someone seeking comfortable mobility for daily walks.
Questions to Ask Your Doctor
A conversation with a regenerative medicine specialist is the most important step. To get the most out of your consultation, come prepared with questions. You can ask things like: “Based on my imaging and diagnosis, why is one therapy better for me?” or “What is a realistic timeline for seeing improvement?” It’s also helpful to ask about the recovery process and what you can do to support the best possible outcome. A thorough evaluation is key to creating a personalized treatment plan, so don’t hesitate to schedule a consultation to discuss your specific case and find clarity on your path forward.
Related Articles
- Stem Cell Therapy for Joint Pain & Arthritis Relief | Miami Stem Cell
- What Does PRP for Arthritis Cost? A Full Breakdown – Stem Cell Therapy | Miami Stem Cell
- A2M vs. PRP for Knee Pain: Which Is Best? – Stem Cell Therapy | Miami Stem Cell
Frequently Asked Questions
How do I know if I need PRP or stem cell therapy? The best choice really depends on the extent of your joint damage. Think of PRP as a powerful supporter for your body’s existing repair crew; it’s great for mild to moderate conditions like early arthritis or tendon strains. Stem cell therapy, on the other hand, is like calling in a specialized construction team to rebuild. It’s often the better option for more advanced degeneration or significant cartilage loss where new tissue is needed. A detailed consultation with a specialist is the best way to determine the right path for you.
Are these treatments painful, and what is the downtime? Both procedures involve an injection, so you might feel a brief pinch, similar to a standard shot. Afterward, it’s common to have some soreness and swelling at the injection site for a few days. This is a positive sign that your body’s healing response has been activated. We typically recommend resting the joint and avoiding strenuous activity for a week or two, but most people can return to their daily routines very quickly.
How long will it take to feel a difference after the treatment? These treatments work with your body’s natural healing cycle, so results are gradual, not instant. Unlike a cortisone shot that just masks pain, regenerative therapies work to repair tissue at a cellular level. Many patients begin to notice improvements in pain and function within a few weeks, with the full benefits often becoming apparent over the following two to three months as your body continues to heal and regenerate.
Why do you use umbilical cord-derived stem cells instead of my own? We use umbilical cord-derived mesenchymal stem cells (MSCs) because they are incredibly potent and versatile. These cells are young, robust, and have a powerful ability to signal healing and regenerate tissue. Sourcing them from an accredited tissue bank also means you get a high concentration of viable cells without needing an invasive procedure, like a bone marrow aspiration, to harvest your own.
Will my insurance cover these treatments? Currently, most insurance providers consider both PRP and stem cell therapies to be elective procedures, so they are typically not covered. We believe in being completely transparent about costs and will provide you with a detailed breakdown based on your personalized treatment plan. We can also discuss financing options to help make these treatments more accessible.