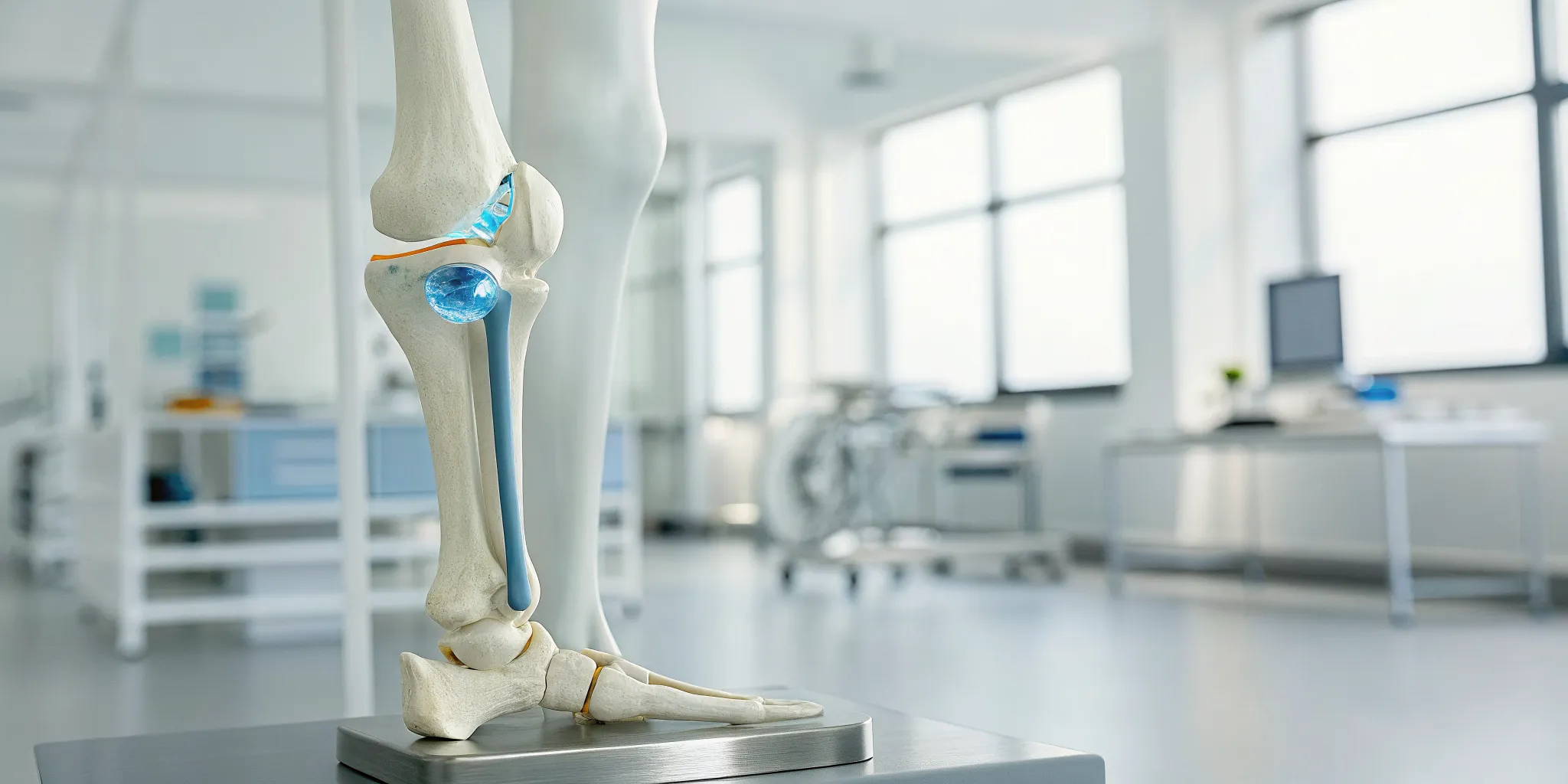
For too long, the approach to severe knee pain has been about managing symptoms. You wait until the pain is unbearable, and then surgery seems like the only answer. Regenerative medicine is changing that conversation. Instead of just putting a bandage on the problem, it focuses on the root cause of joint degeneration. By using your body’s own biological materials, these therapies help reduce inflammation and support the growth of healthier tissue. If you’re looking for real alternatives to surgery for bone on bone, you’re in the right place. We’ll explain how treatments like stem cell therapy work to create a healing environment in your knee for lasting relief.
Key Takeaways
- Prioritize Non-Surgical Solutions First: Before considering knee replacement, build a comprehensive plan using physical therapy, lifestyle changes, and innovative regenerative treatments that can provide lasting relief and help you avoid the operating room.
- Focus on Healing from Within: Unlike temporary fixes like steroid shots, regenerative therapies such as stem cell and exosome treatments work with your body’s natural repair systems to reduce inflammation and rebuild tissue, addressing the root cause of your pain.
- Take Control with Everyday Choices: You can significantly reduce knee pain by making smart lifestyle adjustments. Managing your weight, adopting low-impact exercises, and eating an anti-inflammatory diet create the foundation for long-term joint health.
What Does “Bone-on-Bone” Knee Arthritis Mean?
If you’ve been told you have “bone-on-bone” knee arthritis, it simply means you’re dealing with an advanced stage of osteoarthritis. Think of the cartilage in your knee as a smooth, protective cushion between the ends of your bones. Over time, this cushion can wear down, and when it’s gone, the bones start to rub directly against each other. This friction is what causes the significant pain, stiffness, and swelling that can make everyday activities feel like a challenge. While the diagnosis sounds serious, it’s important to know that it doesn’t automatically mean surgery is your only option. Many effective treatments can help manage your symptoms and improve your quality of life.
What Causes This Type of Knee Pain?
The main reason bone-on-bone arthritis develops is the gradual breakdown of that essential knee cartilage. While it’s often associated with getting older, age is just one piece of the puzzle. Several other factors can contribute to or speed up this process. Previous joint injuries, for instance, can damage the cartilage and make it more vulnerable to wear and tear down the line. Your genetics can also play a role in your predisposition to arthritis. Additionally, carrying excess weight puts more pressure on your knee joints, which can accelerate cartilage deterioration. Understanding these contributing factors can help you and your doctor create a more effective management plan.
Understanding Cartilage Breakdown
Bone-on-bone knee pain is the direct result of osteoarthritis, a condition where the protective cartilage cushioning your knee joint wears away. Imagine it like the tread on a tire—once it’s gone, you’re left with a rough, unprotected surface. This loss of cartilage causes the bones in your joint to rub more closely together, leading to friction, inflammation, and that all-too-familiar deep, aching pain. The goal of effective treatment isn’t just to mask this pain but to address the underlying environment that’s allowing the cartilage to degrade. By focusing on joint regeneration, it’s possible to create conditions that support the health of your remaining cartilage and reduce the inflammation driving your symptoms.
Common Contributing Factors
While wear and tear over time is a major player, several specific factors can accelerate cartilage breakdown. A significant past injury, like a torn meniscus or ACL, can alter the mechanics of your knee and place uneven stress on the cartilage, leading to premature wear. Genetics can also determine the quality of your cartilage and your predisposition to inflammation. Furthermore, carrying excess weight significantly increases the load on your knees with every step you take, which can wear down the cartilage much faster. Recognizing these risk factors is the first step in creating a personalized plan to protect your joints for the long haul.
The Role of Bone Marrow Lesions
Interestingly, the “bone-on-bone” pain you feel might not just be from the surfaces rubbing together. Research shows that much of the discomfort from advanced arthritis actually comes from what’s happening *inside* the bone. These are often called “bone marrow lesions” (BMLs), which are essentially small stress fractures or bruises within the bone just beneath the cartilage. When the cartilage cushion is gone, the bone underneath absorbs more shock than it’s designed to handle, leading to these painful lesions. This is a critical point because treatments that only focus on the joint space might miss the true source of your pain. Advanced regenerative therapies, however, work on a cellular level to reduce inflammation and support healing in both the cartilage and the underlying bone.
Symptoms to Watch For and What to Expect Over Time
Living with bone-on-bone knee arthritis often involves a distinct set of symptoms. You might feel a deep, aching pain that gets worse when you walk, climb stairs, or stand up after sitting for a while. Stiffness is also very common, especially in the morning or after periods of inactivity. Many people also experience noticeable swelling around the knee and a decreased range of motion, making it difficult to fully bend or straighten the leg. As the condition progresses, these symptoms can become more constant and severe, sometimes leading to chronic pain that interferes with your daily life and mobility.
The Prevalence of Knee Arthritis
If you’re dealing with knee pain, you are far from alone. Knee arthritis is incredibly common, and the numbers might surprise you. Research shows that nearly half of all people—about 45%—have a lifetime risk of developing knee osteoarthritis. When you consider the daily demands placed on our knees, this statistic starts to make a lot of sense. With every step you take, your knees absorb a force equivalent to several times your body weight. Over decades, this cumulative stress, combined with factors like old sports injuries or genetics, can lead to significant cartilage wear. This widespread issue affects millions, highlighting the urgent need for effective treatments that go beyond temporary fixes and address the underlying problem.
Why Surgery Isn’t Your Only Option
Hearing the phrase “bone-on-bone” can make you feel like knee replacement surgery is inevitable, but that isn’t the case. There is a wide range of non-surgical treatments that can provide significant pain relief, reduce inflammation, and improve your knee function. The goal is to find a solution that helps your body heal and manage symptoms without the risks and long recovery time associated with major surgery. Innovative approaches in regenerative medicine, like stem cell therapy and PRP injections, are showing incredible promise in helping people find lasting relief and get back to the activities they love, all while avoiding the operating room.
Effective Non-Surgical Alternatives for Knee Pain
Before you even consider surgery, it’s important to know you have a whole toolkit of effective, non-invasive options available. These strategies focus on reducing pain, improving function, and strengthening your body’s natural support systems. Think of them not as temporary fixes, but as foundational steps toward long-term joint health. By combining a few of these approaches, many people find significant relief and can get back to doing what they love without going under the knife.
Strengthening Your Knees with Physical Therapy
One of the most powerful tools for managing knee pain is physical therapy. A good physical therapist acts as your personal coach, guiding you through exercises designed to strengthen the muscles around your knee. When these muscles—like your quadriceps and hamstrings—are strong, they take a significant amount of stress off the joint itself. It’s not just about lifting weights; it’s about improving your balance, flexibility, and overall movement patterns. This hands-on care and education can make a world of difference in your daily comfort and ability to stay active, forming a critical part of any pain management plan.
Tools and Techniques in Physical Therapy
Your physical therapist will use a variety of techniques tailored to your specific needs. This often includes manual therapy, where the therapist uses hands-on methods to stretch tight tissues and improve joint mobility. You’ll also work through a series of therapeutic exercises designed to correct imbalances and build strength where you need it most. They might also incorporate tools like resistance bands or stability balls to challenge your muscles in a safe, controlled way. The goal isn’t just to make you stronger but to retrain your body to move more efficiently, reducing the daily strain on your knee joint and giving you the confidence to stay active.
Complementary Hands-On Therapies
Beyond physical therapy, other hands-on treatments can complement your recovery. Therapies like massage can help release muscle tension around the knee, while some people find relief through acupuncture or chiropractic adjustments. For those looking for a more advanced approach that targets healing at the cellular level, regenerative medicine offers powerful solutions. Treatments like Platelet-Rich Plasma (PRP) therapy use concentrated platelets from your own blood to create a healing response in the joint. These innovative therapies work to reduce inflammation and support your body’s natural ability to repair damaged tissue, offering a path to lasting relief without surgery.
Smart Strategies for Managing Daily Pain
While medication isn’t a long-term solution, it can play a key role in managing flare-ups and reducing inflammation so you can participate in other treatments like physical therapy. Over-the-counter anti-inflammatories can help take the edge off, but your doctor might also discuss injections. Corticosteroid shots can offer fast, temporary relief from severe inflammation. For a more regenerative approach, many people turn to Platelet-Rich Plasma (PRP) therapy. This treatment uses a concentration of your own blood platelets to help encourage your body’s natural healing processes right at the source of the pain.
Over-the-Counter Medications
When knee pain flares up, reaching for an over-the-counter pain reliever is often the first step. It’s helpful to know the difference between your options. Nonsteroidal anti-inflammatory drugs (NSAIDs), like Motrin or Advil, are designed to tackle both pain and swelling, making them a good choice when your knee feels puffy and inflamed. On the other hand, acetaminophen, the active ingredient in Tylenol, focuses solely on reducing pain. This can be a better option for individuals who need to be mindful of kidney health or who aren’t dealing with significant swelling. While these medications can provide necessary short-term relief, they don’t address the underlying cause of cartilage breakdown.
A Warning About Narcotic Painkillers
It’s crucial to draw a clear line between managing chronic pain and using heavy-duty medications. Strong painkillers known as narcotics or opioids, such as hydrocodone, are not intended for the long-term management of arthritis. These medications carry a significant risk of addiction and are best reserved for severe, short-term pain, like what you might experience immediately following a major surgery. For chronic conditions like bone-on-bone knee pain, relying on narcotics can create more problems than it solves. The goal should always be to find sustainable solutions that promote healing and function, rather than simply masking the pain with potentially dangerous drugs.
Joint and Herbal Supplements
Many people explore supplements like glucosamine and chondroitin to support their joint health. These compounds are naturally found in healthy cartilage, where they act as building blocks and help maintain its structure. The idea behind taking them as a supplement is to slow down cartilage deterioration and reduce discomfort. While research has shown mixed results, some studies suggest that high doses of these supplements have helped a significant number of people reduce their pain. It’s not a guaranteed fix for everyone, but for some, it can be a valuable part of a broader strategy to manage knee arthritis symptoms without resorting to more invasive measures.
At-Home Therapies for Relief
You have more power over your knee pain than you might think, and simple at-home strategies can make a big impact. Gentle, consistent movement is key. Activities that don’t jolt your joints, such as walking on flat ground, using a stationary bike, or performing exercises in a pool, can strengthen supporting muscles and improve flexibility without causing pain. Additionally, don’t underestimate the power of temperature therapy. Applying a heating pad can soothe stiffness and relax muscles, while using a cold pack is excellent for reducing swelling and numbing sharp pain after activity. Integrating these simple habits into your daily routine can provide consistent relief.
Finding Stability with Braces and Supportive Devices
Sometimes your knee just needs a little extra support, and that’s where bracing comes in. A knee brace can help stabilize the joint, improve alignment, and limit painful movements, giving the area a chance to rest and heal. For days when the pain is more intense, using a cane or walker can offload some of your body weight from the affected knee, providing immediate relief. A physical therapist can also help you make small adjustments to your gait—the way you walk—to reduce joint stress with every step you take. These simple tools can make a huge impact on your mobility and independence.
How Much Support Can Assistive Devices Provide?
Think of assistive devices as your knee’s personal support system. A well-chosen knee brace can provide crucial stability, especially if your joint feels weak or gives way. It works by gently compressing the area and guiding your knee through a more stable range of motion, which can significantly reduce pain during activity. For days when the pain is more severe, a cane or walker can be a game-changer. By transferring some of your body weight off the affected knee, these tools provide instant relief and can help you walk more comfortably and safely, reducing the risk of a fall and allowing you to maintain your independence while pursuing other treatments.
The Importance of a Professional Fitting
Grabbing any brace off the shelf might seem like a quick fix, but an ill-fitting device can sometimes do more harm than good. That’s why getting guidance from a professional, like a physical therapist, is so important. They can assess your specific condition and recommend the right type of support for your needs. More importantly, they will ensure it fits correctly and teach you how to use it properly. A professional can also analyze your gait—the way you walk—and suggest small adjustments that reduce joint stress with every step. Getting this expert advice is a key part of a comprehensive pain management strategy and ensures these simple tools have the maximum positive impact on your mobility.
Modify Your Activities, Not Your Life
This isn’t about giving up your favorite hobbies; it’s about finding smarter ways to enjoy them. One of the most impactful changes you can make is managing your weight. Every extra pound you carry puts several extra pounds of pressure on your knees. Losing even 10% of your body weight can cut your knee pain significantly. It also means being mindful of activities that cause pain to flare. Instead of high-impact running, you might try swimming or cycling. It’s about listening to your body and choosing activities that build you up without breaking you down, supporting your overall wellness goals.
Correcting Your Stride with Foot and Ankle Orthotics
It might sound strange, but sometimes the source of your knee pain isn’t your knee at all—it’s your feet. The way your feet hit the ground affects everything up the chain, including your ankles, knees, and hips. If you have issues like flat feet or poor alignment, it can throw off your entire stride, causing uneven pressure and stress on your knee joints with every step. This is where custom foot and ankle orthotics can be a game-changer. These aren’t the flimsy inserts you find at the drugstore; they are specially designed to correct your specific alignment issues. By providing the right support, orthotics help distribute your weight more evenly and improve your overall biomechanics. This simple correction can take a significant load off your knees, reducing pain and helping to create a more stable foundation for all your movements as part of a comprehensive plan for joint regeneration.
How Effective Are Knee Injections?
If you’re dealing with bone-on-bone knee pain, you’ve likely heard about injections as a way to find relief without going under the knife. It’s a popular middle-ground treatment, but it’s important to know that not all injections are created equal. They range from temporary symptom-maskers to treatments designed to support your body’s own healing processes.
Understanding the differences is key to choosing a path that aligns with your long-term health goals. Some injections offer quick, short-term relief, which can be a lifesaver for managing a painful flare-up. Others, like platelet-rich plasma (PRP) therapy, take a more regenerative approach by using your body’s own growth factors to address the underlying issue. Let’s walk through the most common options so you can see how they stack up and what might be the best fit for you.
The Pros and Cons of Corticosteroid Injections
Corticosteroid injections are often one of the first options people try for knee arthritis. They work by delivering a powerful anti-inflammatory medication directly into the joint, which can reduce pain and swelling quite effectively. For many, this brings welcome relief that can last for several weeks, making daily activities more manageable.
However, it’s important to view corticosteroids as a short-term solution. Some studies raise concerns about their long-term use, suggesting they may contribute to cartilage loss over time without offering significant pain improvement after a couple of years. While they still have a place in pain management for immediate relief, they don’t address the root cause of joint degeneration. Think of them as a temporary patch, not a long-term repair.
Hyaluronic Acid: A Lubricant for Your Knees?
Think of hyaluronic acid as the natural lubricant and shock absorber for your joints. Your body produces it on its own, but levels can decrease in an arthritic knee. Hyaluronic acid injections aim to supplement this loss, helping to cushion the joint, reduce friction, and ease pain. This approach is less about fighting inflammation and more about restoring a healthier joint environment.
Unlike a one-and-done steroid shot, treatment with hyaluronic acid often involves a series of injections over a few weeks before you feel the full effect. It’s a gentler approach that can provide relief for several months, but it’s still a supportive measure rather than a regenerative one. It helps manage symptoms but doesn’t actively repair the damaged tissue.
How PRP Therapy Helps Your Body Heal Itself
Platelet-Rich Plasma (PRP) therapy is where we shift from simply managing symptoms to actively promoting healing. This treatment uses a concentration of your own blood platelets, which are rich in growth factors that signal your body to repair damaged tissue. The process is straightforward: a small sample of your blood is drawn, spun in a centrifuge to isolate the platelets, and then injected back into your knee.
Because PRP therapy uses your own biological material, it is generally considered very safe. The most common side effects are mild and temporary, like some initial soreness or inflammation at the injection site as the healing process kicks in. It’s a powerful way to support your body’s natural ability to heal from within.
What Are the Risks of Knee Injections?
When considering any injection, it’s natural to think about the potential downsides. With corticosteroids, risks can include infection (though rare), damage to nearby tissues, and the cartilage degradation we mentioned earlier. Hyaluronic acid carries a small risk of a temporary inflammatory reaction, sometimes called a “pseudo-septic” reaction.
Regenerative treatments like stem cell therapy tend to have a strong safety profile. Side effects are typically mild and short-lived, such as temporary swelling, stiffness, or discomfort at the injection site that usually resolves within a week. Studies show that major complications are very rare, making it a reassuring option for those looking for a treatment that works with their body, not against it. For more detailed information, you can always review our FAQs.
Beyond Injections: What’s New in Knee Treatment?
If you’re looking for treatments that go beyond managing symptoms, regenerative medicine is where the most exciting progress is happening. This field focuses on harnessing your body’s own healing mechanisms to repair and restore damaged tissue. Instead of just masking pain, the goal is to address the root cause of joint degeneration. For bone-on-bone knee pain, this means finding ways to reduce inflammation, protect remaining cartilage, and support the growth of new, healthy tissue.
These therapies represent a significant shift in how we approach chronic conditions like osteoarthritis. By using powerful biological materials like stem cells and exosomes, regenerative medicine offers a path toward lasting relief and improved function without the need for invasive surgery. It’s about working with your body to rebuild what’s been lost to wear and tear, giving you a chance to get back to the activities you love with less pain and more confidence.
How Umbilical Cord-Derived Stem Cells Work
You’ve likely heard about stem cells, but it’s helpful to know what makes them so special for joint health. Umbilical cord-derived mesenchymal stem cells (MSCs) are particularly powerful. These cells are collected from the umbilical cord lining after a healthy birth, a process that is completely non-invasive and safe for both mother and baby.
What makes these MSCs so effective is their incredible versatility. They act as the body’s master repair crew. When introduced into an arthritic knee, they can help orchestrate a healing response. They release anti-inflammatory signals to calm the painful inflammation cycle and can encourage your own cells to begin the repair process. This approach supports joint regeneration from within, helping to create a healthier environment inside the knee.
What Is Exosome Therapy and How Can It Help?
Think of exosomes as the messengers of the cellular world. They are tiny vesicles released by stem cells that carry important instructions—like proteins and genetic information—to other cells. In essence, they deliver the “how-to” guide for healing directly where it’s needed. Exosome therapy isolates these powerful communicators and uses them to direct the repair process in your knee.
When used for knee arthritis, exosomes can tell your cells to reduce inflammation and start rebuilding damaged tissue. Because they are so small, they can travel easily and efficiently to facilitate cell-to-cell communication. This therapy is a highly targeted way to leverage the healing power of stem cells without using the cells themselves, offering a sophisticated method for promoting natural tissue repair and pain relief.
What Is Genicular Artery Embolization (GAE)?
Another innovative, minimally invasive procedure gaining attention is Genicular Artery Embolization (GAE). This treatment takes a different approach by targeting the inflammation process from another angle. In an arthritic knee, there is often an overgrowth of tiny blood vessels in the joint lining, which contributes to chronic inflammation and pain.
GAE works by blocking these specific blood vessels. A specialist injects microscopic beads into the arteries supplying the inflamed joint lining, reducing blood flow to those areas. This calms the inflammation, which in turn provides significant pain relief. While it doesn’t rebuild cartilage, GAE is being studied as a promising alternative for those who aren’t ready for or don’t want a knee replacement.
Who Is a Good Candidate for GAE?
Genicular Artery Embolization is a particularly good option for people with moderate to severe knee osteoarthritis who feel like they’ve tried everything else without success. It’s also a valuable alternative for those who aren’t candidates for a full knee replacement, whether due to age or other health concerns like heart disease or diabetes. If you’re looking for meaningful pain relief but want to avoid a major operation, GAE could be a fitting choice. It bridges the gap between conservative treatments that are no longer working and the commitment of a total joint replacement, offering a minimally invasive path to feeling better.
What Recent Studies Show
What’s really exciting about GAE is that its benefits may go beyond simple pain relief. Early research suggests that by reducing the chronic inflammation in the knee, the procedure might also help slow down the progression of the arthritis itself. This is a significant development because it shifts the goal from just managing symptoms to potentially preserving the long-term health of your joint. While more research is always ongoing, these findings offer hope that GAE could be a way to not only improve your quality of life now but also protect your knee’s function for the future.
Subchondroplasty (SCP): A Minimally Invasive Option
Another procedure to know about is Subchondroplasty, or SCP. This is a minimally invasive surgery designed to address a specific source of knee pain: bone marrow lesions. Think of these as small stress fractures or deep bruises in the bone beneath your cartilage. They can be incredibly painful and often show up on an MRI. During an SCP procedure, a surgeon injects a bone-substitute material into these lesions. This material hardens and supports the bone, helping it heal from the inside out and relieving the pain associated with the lesion.
SCP is often a great fit for active people who are dealing with significant pain but want to avoid the long recovery and activity restrictions that come with a total knee replacement. Because it targets a very specific problem within the bone, it can provide substantial relief while preserving your natural joint. It’s a strategic repair job rather than a full replacement, making it an appealing option for those who want to get back to their lives more quickly without the limitations of a traditional knee surgery.
Regenerative vs. Traditional: Which Is Right for You?
When you place regenerative therapies alongside traditional treatments, the fundamental difference in approach becomes clear. Injections like corticosteroids offer fast, temporary relief by suppressing inflammation, but they don’t address the underlying cartilage damage. In fact, repeated steroid use can sometimes weaken cartilage over time.
Regenerative options, on the other hand, are designed to create lasting change. Therapies using stem cells and exosomes aim to alter the environment within the joint, shifting it from a state of chronic breakdown to one of active repair. Patients often experience not just significant pain relief but also improved function. By supporting your body’s innate ability to heal, these treatments for arthritis can provide a more sustainable solution for managing bone-on-bone knee pain.
What Lifestyle Changes Can Reduce Your Knee Pain?
While advanced regenerative treatments can be transformative, the small choices you make every day have a massive impact on your knee health. Think of lifestyle adjustments as the foundation that supports any clinical therapy you pursue. By making strategic changes to your diet, exercise routine, and weight, you can actively reduce inflammation, decrease the load on your joints, and build a stronger support system for your knees. These habits work hand-in-hand with treatments like PRP therapy to create lasting relief and improve your overall quality of life. It’s about taking control and giving your body the best possible environment to heal.
Lighten the Load: How Weight Affects Your Knees
It might sound simple, but managing your weight is one of the most effective things you can do for your knees. Here’s a powerful way to think about it: for every extra pound of body weight you carry, your knees experience about four pounds of added pressure when you walk or climb stairs. That pressure adds up, accelerating wear and tear on your cartilage. Losing even a small amount of weight can significantly lighten that load, leading to less pain and improved function. This isn’t about a drastic diet; it’s about making sustainable changes that reduce stress on your joints and decrease the body-wide inflammation that contributes to arthritis pain.
The Direct Impact of Weight on Knee Pressure
It’s easy to underestimate the connection between your weight and your knee pain, but the numbers are striking. For every extra pound of body weight you carry, your knees are forced to endure about four extra pounds of pressure with every step you take. That force multiplies when you do things like climb stairs or stand up from a chair. This constant, excess load acts like a grinding force on your cartilage, speeding up its deterioration and worsening inflammation. The good news is that this works in reverse, too. Losing even a modest amount of weight can dramatically lighten that load, providing significant pain relief and slowing down the progression of arthritis. It’s one of the most direct ways you can take control of your joint health.
How a Healthy Weight Improves Surgical Outcomes
Even if your primary goal is to avoid surgery, managing your weight is a smart strategy that prepares you for any possibility. Should you eventually need a knee replacement, being at a healthier weight significantly improves your chances of a smooth recovery and a successful long-term outcome. Studies show that overweight patients have a much higher risk of complications like infection after joint replacement surgery. A healthy weight also helps new joints last longer by reducing the daily stress placed on them. Think of it as an investment in your future health—one that pays off whether you end up in the operating room or successfully manage your pain with regenerative treatments.
Exploring Medical Weight Loss Programs
If you’ve tried to lose weight on your own without success, you’re not alone. A medical weight loss program offers a structured, supportive approach that goes beyond simple diet and exercise. These programs are supervised by healthcare professionals who can create a personalized plan tailored to your body and your goals. This might include strategies like appetite-curbing medications to help you manage cravings or vitamin injections to support your metabolism and energy levels. By partnering with a professional, you can safely and effectively lose weight, which is a critical step in reducing the stress on your knees and improving your overall longevity plan.
Strengthen Your Knees with Low-Impact Exercise
When your knees hurt, your first instinct might be to stop moving. However, the right kind of movement is essential for long-term joint health. The goal is to strengthen the muscles that support your knee—particularly your quadriceps and hamstrings—without putting stress on the joint itself. Stronger muscles act like a natural brace, absorbing shock and stabilizing the knee. Low-impact exercises are perfect for this. Activities like swimming, cycling on a stationary bike, or simply going for a walk allow you to build strength and improve your range of motion without the jarring impact of running or jumping. Consistency is key to seeing real improvement.
Fight Inflammation with Your Fork
The food you eat can either fuel inflammation or fight it. For knee arthritis, which is an inflammatory condition, your diet is a powerful tool. An anti-inflammatory diet focuses on whole, nutrient-dense foods that help calm your body’s inflammatory response. Fill your plate with colorful fruits and vegetables, lean proteins like fish and chicken, and healthy fats from sources like avocados, nuts, and olive oil. At the same time, try to limit processed foods, sugary drinks, and refined carbohydrates, as these can trigger inflammation and make your symptoms worse. This approach doesn’t just help your knees; it supports your overall anti-aging and wellness goals.
Take the Pressure Off with Water-Based Exercise
If land-based exercise feels too painful, the pool can be your best friend. Water-based exercise, or aquatic therapy, is incredibly beneficial for people with bone-on-bone knee pain. The natural buoyancy of water supports your body weight, which takes nearly all the pressure off your aching joints. This allows you to move more freely and with less pain than you could on land. At the same time, the water provides gentle resistance, helping you build muscle strength and improve flexibility. Whether you’re swimming laps, walking in the shallow end, or joining a water aerobics class, you’re getting an effective workout without the painful impact.
How Do You Choose the Right Treatment Path?
Deciding on the best way to treat your bone-on-bone knee pain is a deeply personal choice. With so many options available, from physical therapy to advanced regenerative medicine, it’s easy to feel overwhelmed. The key is to find a path that aligns with your body, your lifestyle, and your long-term health goals. Surgery is a major step, and it’s not always the first or best one. Exploring non-surgical alternatives gives you the power to make an informed decision that feels right for you.
Think of this as building a personalized roadmap to recovery. It involves understanding your specific condition, weighing the practical aspects like cost and recovery time, and working with a medical professional to create a comprehensive plan. Let’s walk through the key considerations to help you find your way forward.
What to Consider When Choosing a Treatment
The right treatment for you depends on several personal factors. The severity of your arthritis, your age, and your overall health all play a significant role in determining the most effective approach. For instance, a treatment that works for a highly active 50-year-old might differ from the best option for someone who wants to enjoy gardening without pain. It’s essential to have a candid conversation with a healthcare professional to discuss your options and create a plan tailored to your unique situation. Your personal goals are also a huge part of the equation. Are you aiming to get back to a specific sport, or is your main objective to walk up the stairs without wincing? Being clear about what you want to achieve will help guide your treatment decisions.
Will Insurance Cover Non-Surgical Treatments?
Navigating the financial side of healthcare can be tricky. While knee replacement surgery is typically covered by insurance, many effective non-surgical alternatives may not be. It’s important to check with your provider to understand what your plan covers. Regenerative treatments, for example, are often paid for out-of-pocket. However, it’s helpful to view these therapies as an investment in your long-term well-being. When you factor in the costs of a hospital stay, extensive rehabilitation, and time away from work associated with surgery, non-surgical options can be a financially sound choice. You can learn more by reviewing our patient testimonials to see how others have valued this investment in their health.
Building Your Personalized Treatment Plan
The most successful outcomes often come from a multi-faceted approach rather than a single solution. Combining different therapies can create a powerful synergistic effect that supports your body’s healing process from all angles. For example, a regenerative treatment like stem cell therapy can work to repair damaged cartilage at a cellular level, while a physical therapist can design a specialized exercise plan to strengthen the muscles supporting your knee joint. This combination reduces stress on the joint and improves stability. Adding lifestyle adjustments, such as an anti-inflammatory diet, can further enhance your results. A comprehensive plan addresses your immediate pain while also building a foundation for lasting joint health.
Setting Realistic Expectations for Your Recovery
Understanding the recovery process is crucial when comparing your options. Knee replacement surgery involves a significant recovery period, often including a hospital stay followed by weeks or months of intensive physical therapy. In contrast, non-surgical treatments offer a much different experience. Injections like cortisone can provide temporary relief for a few months, but they don’t heal the underlying issue. Regenerative therapies at Miami Stem Cell focus on long-term healing with minimal downtime. While you won’t see results overnight, patients typically notice gradual improvement as their bodies begin to repair and regenerate tissue over several weeks and months. This approach allows you to get back to your life faster, without the long and painful interruption of surgery.
Related Articles
- 7 Alternatives to Knee Replacement Surgery
- A2M vs. PRP for Knee Pain: Which Is Best?
- Stem Cell Therapy for Joint Regeneration: Relief for Pain
Frequently Asked Questions
How long does it take to see results from regenerative treatments like stem cell therapy? Unlike a corticosteroid shot that provides quick, temporary relief, regenerative therapies work with your body’s natural healing timeline. This means the results are gradual. Most people begin to notice improvements in pain and function within a few weeks, with the most significant changes often occurring over the following two to three months as your body’s cells work to repair the damaged tissue.
What makes someone a good candidate for these non-surgical treatments? Generally, the best candidates are individuals who are dealing with chronic knee pain from osteoarthritis and want to find a lasting solution that avoids the risks and long recovery of a knee replacement. If you’re looking to improve your quality of life and get back to your activities without major surgery, these treatments are worth exploring. The only way to know for sure is to have a thorough consultation to assess your specific condition and health goals.
Is there a difference between PRP and stem cell therapy for knee pain? Yes, they work in slightly different ways. Think of Platelet-Rich Plasma (PRP) therapy as a way to amplify your body’s own healing signals. It uses a concentration of your own platelets to encourage repair. Stem cell therapy, particularly with umbilical cord-derived cells, introduces a powerful new team of cells that can orchestrate a more comprehensive healing response, making it a more robust option for advanced conditions like bone-on-bone arthritis.
Are regenerative procedures like stem cell injections painful? You can expect some discomfort, similar to what you’d feel with any injection. We use a local anesthetic to numb the area, so the procedure itself is very tolerable. You might feel some soreness or stiffness in the knee for a day or two afterward, which is a normal sign that the healing process is beginning. This is very different from the significant post-operative pain and rehabilitation required after a knee replacement.
Why are most regenerative therapies not covered by insurance? Because these treatments are at the forefront of medical science, they are still considered relatively new by insurance companies, which can be slow to adapt. As a result, they haven’t been assigned the standard billing codes needed for coverage. Many people view this as an investment in their long-term health, allowing them to avoid the costs, downtime, and potential complications associated with major surgery.