If you’ve started researching solutions for joint pain, you’ve probably been flooded with conflicting information. One article recommends a miracle supplement, while another insists that surgery is the only real answer. It’s enough to make anyone feel overwhelmed and unsure of where to turn. The truth is, effective cartilage care isn’t about a single quick fix; it’s about creating a comprehensive strategy tailored to your body. We’re here to cut through the noise and provide a clear, straightforward look at your options. We’ll debunk common myths and explain the best treatments for cartilage protection, helping you understand how regenerative medicine, physical therapy, and smart lifestyle choices work together to preserve your joints for the long haul.
Key Takeaways
- Proactive care is non-negotiable for cartilage health: Your cartilage lacks the blood supply needed to heal itself, so ignoring joint pain allows damage to progress. Addressing issues early is the most effective way to protect your long-term mobility.
- Regenerative medicine is a powerful, non-surgical solution: Therapies like stem cell and PRP therapy work with your body’s natural healing systems to repair tissue and reduce inflammation. This approach addresses the root cause of joint pain, helping you recover without the risks and downtime of surgery.
- A personalized strategy is your best defense against joint pain: The most effective plans combine smart lifestyle habits, like weight management and low-impact exercise, with a professional treatment strategy. Consulting a specialist helps you create a comprehensive approach tailored to your specific condition and goals.
What Is Cartilage (And Why Does It Matter)?
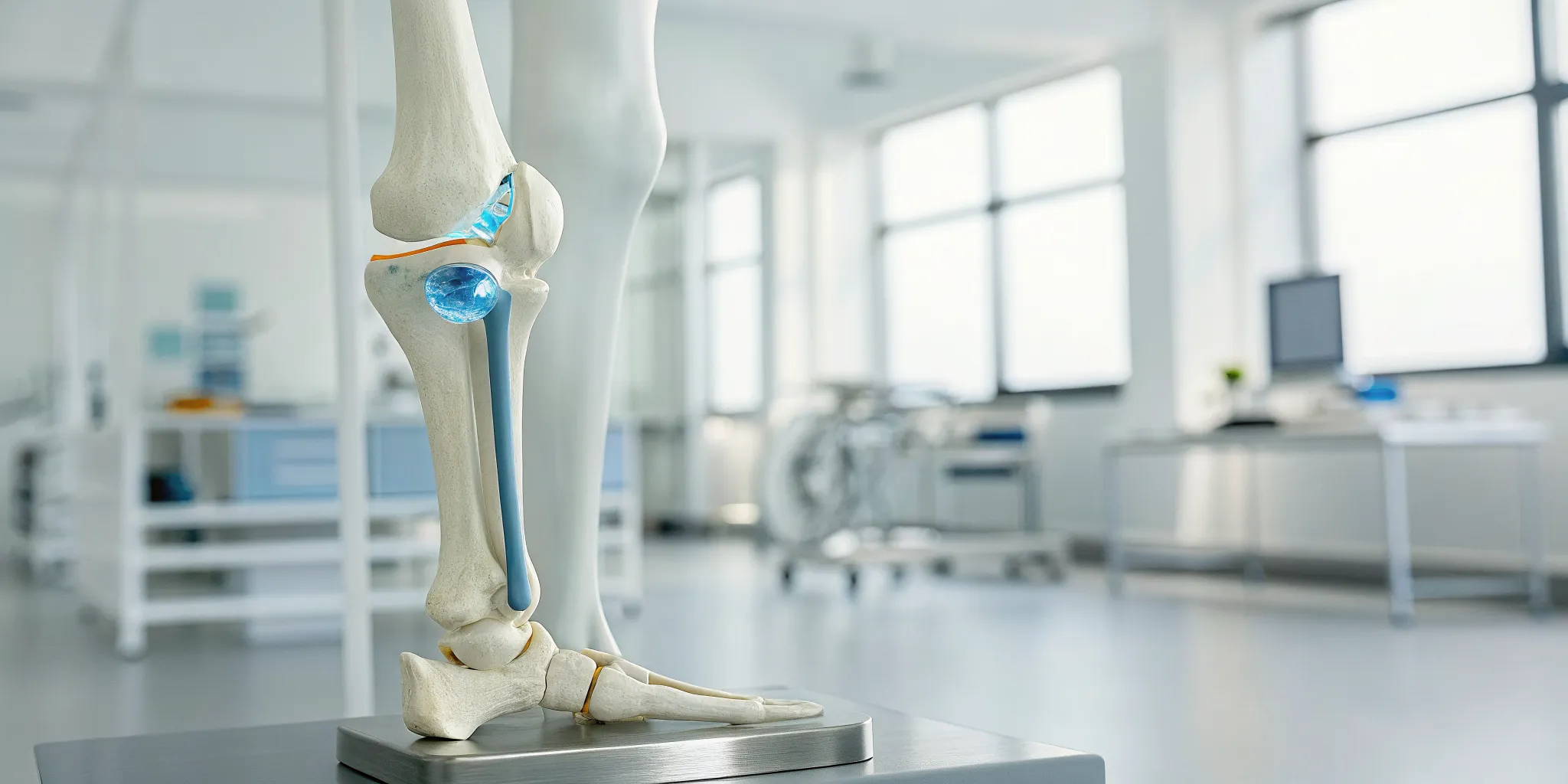
Think of cartilage as the unsung hero of your joints. It’s a firm, flexible connective tissue that keeps your bones from grinding against each other. You can find it throughout your body, from your ears and nose to your rib cage, but it plays an especially critical role in your joints. This vital tissue acts as a protective cushion, absorbing shock and ensuring your movements are smooth and pain-free.
When your cartilage is healthy, you probably don’t give it a second thought. You can walk, run, and move with ease. But when it starts to wear down from injury, age, or disease, the effects can be debilitating. Understanding what cartilage is and how it works is the first step toward protecting your joints for the long haul and exploring effective treatments that go beyond just managing symptoms. At Miami Stem Cell, we focus on addressing the root cause of joint pain, which often begins with the health of your cartilage.
The Cushion for Your Joints
The specific type of cartilage in your joints is called articular cartilage. According to experts at Yale Medicine, “Articular cartilage is a tough, flexible tissue that covers the ends of bones in joints like the knee, elbow, hip, and ankle. It helps bones slide smoothly against each other.” This slick, slippery surface allows for a wide range of motion with minimal friction. It also distributes weight and absorbs impact during physical activities, protecting the underlying bone from stress. This cushioning effect is essential for maintaining healthy joint regeneration and preventing the pain and stiffness that can limit your lifestyle.
What Happens When Cartilage Wears Down
One of the biggest challenges with cartilage is that it has a very limited ability to heal itself. As researchers note, “When this cartilage gets damaged (from injury, overuse, or diseases like osteoarthritis), it’s hard for it to heal on its own because it doesn’t have blood vessels.” Without a direct blood supply, the cells needed for repair can’t reach the damaged area. This is why a cartilage injury that seems minor at first can lead to chronic pain and dysfunction. If left unaddressed, the damage can worsen over time, leading to conditions like arthritis and, in severe cases, the potential need for joint replacement surgery.
What Causes Cartilage to Break Down?
Think of your cartilage as the unsung hero of your joints. This smooth, resilient tissue works tirelessly to cushion your bones and allow for fluid, pain-free movement. But it’s not invincible. Over time, several factors can contribute to its breakdown, leading to stiffness, pain, and reduced mobility. Understanding these causes is the first step toward protecting your joints for the long haul. It’s rarely one single event but often a combination of lifestyle, genetics, and life events that leads to cartilage damage.
Everyday Wear and Tear
Just like the tread on a tire, your cartilage can wear down from years of use. Every step, bend, and twist contributes to this gradual process. While this is a natural part of aging, certain high-impact activities or repetitive motions can speed it up. This slow, steady erosion is what we often see in osteoarthritis, where the protective cartilage thins out over time. This type of joint degeneration is incredibly common, but that doesn’t mean you have to accept the discomfort that comes with it. Recognizing the impact of daily life on your joints helps you make smarter choices about activity and recovery.
Injuries and Trauma
A sudden injury from a fall, a sports accident, or another form of trauma can cause immediate and significant damage to your cartilage. A hard hit or a sharp twist can create tears or defects in the smooth cartilage surface. The real problem is that cartilage has a very limited ability to heal itself because it lacks a direct blood supply. This means that even a small injury can create a weak spot that worsens over time, eventually leading to more widespread damage and chronic pain. This is why addressing joint injuries properly from the start is so critical for long-term health.
Excess Weight and Joint Stress
Carrying extra weight places a tremendous amount of stress on your weight-bearing joints, especially your hips, knees, and ankles. It’s a matter of simple physics: with every step you take, your knees support a force multiple times your body weight. When you carry extra pounds, that force increases exponentially, accelerating the breakdown of cartilage. This constant pressure can wear down the protective tissue much faster than it would otherwise. Maintaining a healthy weight is one of the most effective things you can do to reduce joint stress and preserve your cartilage for years to come. Your overall joint health depends heavily on managing this load.
Autoimmune Disorders
Sometimes, the threat to your cartilage comes from within. In autoimmune disorders, the body’s immune system mistakenly attacks its own healthy tissues. For people with conditions like rheumatoid arthritis, the immune system targets the lining of the joints (the synovium), causing inflammation that can eventually destroy both cartilage and bone. Unlike the mechanical wear and tear of osteoarthritis, this type of cartilage damage is driven by a systemic inflammatory process. Managing the underlying autoimmune condition is key to protecting the joints from further destruction and preserving function.
Signs Your Cartilage Needs Attention
Our bodies are great at sending signals when something isn’t right, but it’s easy to dismiss subtle joint aches and pains as a normal part of life. When it comes to your cartilage, however, these early whispers can turn into loud alarms if ignored. Paying attention to how your joints feel and function is the first step in protecting them for the long haul. Understanding these signs can help you take proactive steps to address the root cause, often long before more invasive measures become necessary.
Early Warning Signs of Damage
Think about how your joints feel day-to-day. Do you hear a crackling or popping sound when you bend your knees? Maybe you feel a slight “catching” sensation or a moment of instability when you stand up. These are common early indicators of cartilage damage. Other signs include persistent pain, swelling, stiffness, or a noticeable decrease in your range of motion. If you find you can’t fully bend or straighten a joint like you used to, that’s a clear signal. Ignoring these symptoms can lead to more significant issues, including chronic pain and problems with joint regeneration.
When to See a Specialist
If any of those warning signs sound familiar, it’s time to listen to your body. While it might be tempting to wait and see if the problem resolves itself, cartilage damage doesn’t heal on its own and can worsen over time, potentially leading to osteoarthritis. The good news is that catching it early opens up a world of effective, non-surgical treatment options. Consulting with a specialist doesn’t automatically mean you’re heading for surgery. In fact, many experts prioritize conservative approaches first. A thorough evaluation can give you a clear diagnosis and a personalized plan to protect your joints. The best way to understand your options is to schedule a consultation and get expert guidance.
How to Protect Cartilage Without Surgery
If you’re dealing with joint pain, the idea of surgery can be daunting. The good news is that there are powerful, non-surgical ways to protect your cartilage and get back to feeling your best. These approaches focus on reducing stress on your joints and using your body’s own healing mechanisms to repair damage. Let’s walk through some of the most effective strategies available today.
Stem Cell and Regenerative Therapies
This is where modern medicine gets really exciting. Regenerative therapies use your body’s natural healing abilities to address the root cause of cartilage damage. For instance, stem cell therapy introduces powerful, specialized cells to the injured area. These cells can help reduce inflammation and signal your own tissues to begin repairing themselves. Clinical studies show that for mild to moderate cartilage damage, this approach can lead to significantly less pain and better joint function. It’s a way to work with your body, not against it, to encourage genuine healing and long-term relief.
Platelet-Rich Plasma (PRP) Therapy
You might have heard of athletes using PRP, and for good reason. Platelet-Rich Plasma (PRP) therapy is a treatment that uses a concentrated sample of your own blood. This sample is rich in platelets and growth factors, which are the essential components your body uses to heal injuries. When injected into a damaged joint, PRP can kickstart the repair process, reduce painful inflammation, and promote the healing of cartilage and surrounding tissues. It’s a straightforward and effective way to give your joints the resources they need to recover without invasive procedures.
Hyaluronic Acid Injections
Think of hyaluronic acid as the natural lubricant for your joints. It’s a substance your body already produces to keep things moving smoothly and absorb shock. As we age or experience joint damage, the amount of this fluid can decrease, leading to pain and stiffness. Hyaluronic acid injections supplement your body’s natural supply, helping to cushion the joint and restore smoother movement. While it doesn’t regenerate cartilage, it can provide significant pain relief and improve function, making it a valuable part of a comprehensive pain management plan for many people dealing with osteoarthritis.
Physical Therapy and Smart Exercises
Movement is medicine, especially when it’s done correctly. Physical therapy is a cornerstone of protecting your cartilage because it strengthens the muscles that support your joints. When these muscles are strong, they take a lot of the pressure and stress off the cartilage itself. A good physical therapist can design a program that improves your range of motion, reduces pain, and teaches you how to move in ways that protect your joints from further damage. Combining targeted exercises with other treatments creates a powerful strategy for long-term joint health and stability.
The Role of Weight and Nutrition
It’s a simple fact of physics: extra body weight puts extra stress on your joints, particularly your knees and hips. This constant pressure can speed up the breakdown of cartilage. Losing even a small amount of weight can make a huge difference in reducing that load and easing pain. Paired with a nutrient-rich diet full of anti-inflammatory foods, weight management is one of the most impactful lifestyle changes you can make for your joints. It’s a foundational step that supports any other treatment you pursue and helps protect your cartilage for years to come.
How Regenerative Medicine Repairs Cartilage
Regenerative medicine offers a completely different way of thinking about cartilage damage. Instead of just managing symptoms with pain medication or resorting to invasive surgery, these treatments work directly with your body’s natural healing abilities to repair tissue from the inside out. By using powerful biological tools like stem cells and exosomes, we can target the root cause of joint deterioration. This approach focuses on rebuilding what’s been lost and creating a healthier environment within the joint, paving the way for long-term relief and improved function. It’s about giving your body the resources it needs to truly heal itself.
Using Stem Cells to Regenerate Tissue
Think of stem cells as your body’s internal repair crew. Specifically, Mesenchymal Stem Cells (MSCs) are remarkable because they can develop into new cartilage cells when introduced into a damaged joint. But they do more than just rebuild; they also release powerful anti-inflammatory signals that help calm the joint, reducing the pain and swelling that make movement difficult. This dual-action approach not only helps regenerate joint tissue but also creates a healthier, less painful environment where true healing can occur. It’s a targeted strategy that supports your body’s own repair mechanisms.
The Healing Power of Exosomes
If stem cells are the repair crew, exosomes are the project managers. These tiny vesicles act as messengers, carrying vital instructions from one cell to another. In cartilage repair, exosomes released by stem cells tell surrounding tissues to reduce inflammation, protect existing cartilage cells from further damage, and support the new cells being formed. They are crucial for coordinating the healing process, ensuring all the cellular players are working together effectively. This communication is key to a successful and efficient repair, making exosomes a powerful component of modern regenerative therapies.
Understanding FDA-Compliant Treatments
When considering regenerative medicine, safety and quality are paramount. That’s why it’s so important to choose treatments that are FDA-compliant. This means the clinic follows strict federal guidelines for how cellular products are sourced, processed, and administered, ensuring you receive the highest standard of care. At Miami Stem Cell, we exclusively use therapies that adhere to these regulations. Choosing a compliant provider protects you from the risks associated with unregulated clinics. Understanding the difference between overseas vs. USA stem cell treatments is a critical step in making an informed and safe decision about your health.
Is Surgery the Right Option for You?
When you’re dealing with cartilage damage, the conversation often turns to surgery. For a long time, it has been the go-to solution because cartilage doesn’t heal well on its own. But an invasive procedure isn’t your only path forward. Understanding the common surgical options is a great first step in deciding what’s truly best for your body and your long-term health goals. It helps you weigh the pros and cons against less invasive, regenerative approaches that work with your body’s natural healing abilities.
An Overview of Surgical Procedures
Surgical interventions for cartilage are typically designed to do one of two things: relieve symptoms or attempt to repair and restore the damaged tissue. Because articular cartilage has a limited ability to heal itself, these procedures are often seen as the only way to address significant damage. Some surgeries focus on cleaning out the joint or smoothing rough surfaces to reduce pain, while others are more complex, aiming to rebuild the cartilage surface. Each approach comes with its own recovery timeline and success rate, making it important to understand what you’re signing up for before committing to a procedure that requires significant downtime.
Microfracture Surgery
Microfracture is a technique where a surgeon drills tiny holes into the bone beneath the damaged cartilage. The goal is to create a controlled injury that stimulates a healing response, allowing new cartilage to form. While it sounds promising, this method typically produces a type of cartilage called fibrocartilage, which is more like a scar tissue than the original, durable hyaline cartilage. It’s less resilient and often considered a short-term fix, especially for smaller areas of damage. For many, it can provide temporary relief, but it may not be the permanent solution needed to get back to an active lifestyle without limitations.
Osteochondral Transplantation
Often called OATS (Osteochondral Autograft Transplantation), this procedure is a bit like a transplant using your own tissue. A surgeon takes a small, circular plug of healthy cartilage and underlying bone from a non-weight-bearing area of your joint. This plug is then moved and fitted into the damaged area. This technique is generally used for smaller cartilage defects and can create a strong, durable repair with real cartilage. It’s a popular option for active individuals, but it does mean creating a new, albeit minor, injury site where the healthy tissue was harvested from.
Autologous Chondrocyte Implantation
Autologous Chondrocyte Implantation, or ACI, is a more involved, two-step process. First, a surgeon performs a small biopsy to remove a sample of your healthy cartilage cells. These cells are then sent to a lab where they are grown and multiplied over several weeks. In a second surgery, this newly grown sheet of cells is implanted into the damaged area to encourage new cartilage to develop. While technologically advanced, ACI requires two separate procedures and a lengthy recovery period, making it a significant commitment for any patient.
Deciding Between Surgery and Regenerative Options
Choosing between surgery and a non-surgical alternative is a major decision. While surgical procedures can be effective for certain injuries, they are invasive and often come with long recovery periods. On the other hand, many non-surgical treatments have historically focused on managing symptoms rather than addressing the root cause. This is where regenerative medicine changes the game. Therapies using stem cells and exosomes are designed to support your body’s own healing mechanisms, helping to repair tissue and reduce inflammation from the inside out. By weighing the benefits of surgery against the potential of these innovative, minimally invasive joint regeneration therapies, you can make an informed choice that aligns with your health and lifestyle goals.
The Future of Cartilage Regeneration
The world of medicine is making incredible strides in how we approach cartilage damage. For a long time, the focus was on managing pain or replacing joints, but that’s changing. Researchers are now focused on regeneration, finding ways to help the body rebuild the cartilage it has lost. This shift opens up a whole new set of possibilities for people dealing with joint pain and mobility issues. Instead of just putting a bandage on the problem, the goal is to address the root cause by repairing the tissue itself.
This forward-thinking approach combines biology and technology to create solutions that work with your body’s natural healing processes. The field is evolving quickly, with new research and innovative therapies offering hope for more effective, less invasive treatments that could change the way we think about joint health for good. We’re moving beyond temporary fixes and toward long-term solutions that restore function and improve quality of life. This means less reliance on invasive surgeries and more emphasis on harnessing the body’s own power to heal. It’s an exciting time for anyone looking for lasting relief from joint issues.
A Look at Tissue Engineering
One of the most exciting frontiers in cartilage repair is tissue engineering. Think of it as building a biological support system for your joints. This modern approach uses a combination of your body’s own cells, special growth factors, and a supportive material called a scaffold. The scaffold acts like a temporary, 3D framework where new cartilage cells can attach and grow. It provides the perfect structure and environment for the tissue to regenerate, eventually integrating with your existing cartilage to restore the joint’s cushion and function. This method essentially gives your body the blueprint and building blocks it needs to repair itself from the inside out.
Combining Therapies for Better Results
Sometimes, the most effective approach isn’t just one treatment, but a thoughtful combination of therapies. For instance, growth factors are often used to signal cells and direct the healing process. This is the principle behind Platelet-Rich Plasma (PRP) therapy, which uses a concentration of platelets and growth factors from your own blood to reduce inflammation and support tissue repair. When used alongside other techniques, PRP can help create a healing environment within the joint, making it a powerful tool for conditions like knee osteoarthritis. By layering treatments, we can address the problem from multiple angles for a more comprehensive result.
What’s Next in Regenerative Medicine
Cellular therapy is at the heart of the next wave of cartilage treatment. In particular, Mesenchymal Stem Cells (MSCs) are showing incredible promise. These unique cells can be guided to develop into cartilage-producing cells and release substances that promote overall joint health. Early studies have shown that MSCs are safe and that some patients experience positive results for years. Alongside MSCs, researchers are also exploring exosome therapy, which uses the powerful signaling molecules released by stem cells to orchestrate repair and regeneration within the joint, paving the way for even more sophisticated, cell-free treatments.
Cartilage Treatment Myths vs. Facts
When it comes to joint pain and cartilage damage, there’s a lot of conflicting information out there. It can be tough to separate what’s true from what’s just wishful thinking. Let’s clear up a few common misconceptions so you can make informed decisions about your joint health and explore treatments that actually work. Understanding the facts is the first step toward finding real, lasting relief and getting back to the life you want to live.
Myth: Cartilage Can Heal on Its Own
One of the most persistent myths is that if you just rest enough, your cartilage will eventually repair itself. Unfortunately, this isn’t true. Unlike your skin or bones, articular cartilage lacks a direct blood supply, which is essential for carrying the nutrients and cells needed for healing. Without blood flow, the tissue simply can’t regenerate on its own once it’s damaged. This is why a cartilage injury doesn’t just “get better” with time; it often gets progressively worse. Effective joint regeneration requires a proactive approach that helps your body build new, healthy tissue where it can’t on its own.
Fact: The Truth About Supplements
You’ve probably seen countless ads for supplements like glucosamine and hyaluronic acid, promising to rebuild cartilage and cure joint pain. While some of these supplements may offer mild relief from inflammation or discomfort, they do not repair or regrow damaged cartilage. Think of them as a temporary patch, not a permanent fix. True healing involves addressing the root cause of the damage at a cellular level. Relying solely on supplements can delay you from seeking treatments that offer a real solution for long-term joint health. A science-backed approach focuses on regenerative therapies that work with your body’s natural healing mechanisms.
Myth: Non-Surgical Options Are a Last Resort
Many people believe that non-surgical treatments are only for minor pain and that surgery is the only “real” solution for significant cartilage damage. This outdated view often leads people to endure pain for years, waiting until surgery is their only option. The reality is that advanced non-surgical therapies can be incredibly effective, especially when used proactively. Many people also mistakenly believe that physical therapy or exercise will worsen their pain, but guided movement is crucial for joint health. Regenerative medicine isn’t a last resort; it’s a powerful, primary strategy for pain management that can repair tissue and help you avoid invasive procedures altogether.
How to Choose Your Treatment Plan
Deciding on a treatment for cartilage damage isn’t a one-size-fits-all process. The best path forward is unique to you, your body, and your goals. By looking closely at a few key factors, you can work with your doctor to create a plan that feels right and gets you back to living your life with less pain. Here’s what to consider when weighing your options between surgery and regenerative therapies.
Factor in Your Age and Lifestyle
Your age and how active you are play a significant role in determining the most effective treatment. Surgical procedures often have the best outcomes for active individuals under 40 with specific types of injuries, as their bodies tend to recover more quickly. However, surgery also comes with a long and demanding recovery period that doesn’t fit everyone’s life.
Regenerative medicine offers a powerful alternative, especially if you want to avoid significant downtime. These treatments can be a great fit for people of all ages who want to support their body’s natural healing processes. They align perfectly with a proactive approach to health and are a key part of a long-term longevity plan.
Understand the Extent of the Damage
Getting a clear picture of what’s happening inside your joint is the first step. A specialist will use a combination of a physical exam, your medical history, and imaging like X-rays or MRIs to determine the severity of the cartilage damage. This diagnosis is critical because the extent of the wear and tear often points toward the best solution.
Since articular cartilage doesn’t heal well on its own, surgery is frequently recommended for severe damage. For those with mild to moderate cartilage issues, however, studies show that non-surgical treatments can significantly reduce pain and improve joint function. These therapies focus on creating a healing environment, making them an excellent option for effective joint regeneration without the risks of an invasive procedure.
Find the Right Regenerative Medicine Specialist
With so many different treatments available, from physical therapy to advanced cell-based therapies, having an expert guide you is essential. The right specialist won’t just push one option; they will listen to your concerns, assess your specific condition, and help you understand the pros and cons of every path, including both surgical and regenerative routes.
Look for a clinic that prioritizes personalized care and uses science-backed, FDA-compliant treatments. A great specialist will be your partner in health, working with you to develop a strategy that addresses the root cause of your pain and helps you achieve your long-term wellness goals. When you feel confident in your care team, you can feel confident in your treatment plan.
Protect Your Joints for the Long Haul
Thinking about joint health isn’t just for when you’re in pain; it’s about playing the long game. Protecting your cartilage and supporting your joints is an ongoing commitment that pays off in mobility, comfort, and a better quality of life for years to come. The good news is that you don’t have to make drastic, overwhelming changes all at once. Small, consistent adjustments to your daily routine can make a huge difference. By focusing on smart lifestyle choices, mindful movement, and a proactive maintenance plan, you can give your joints the support they need to carry you through all of life’s adventures.
Simple Lifestyle Changes for Joint Health
Let’s start with the basics. Maintaining a healthy weight is one of the most effective things you can do for your joints, as it reduces the daily stress on your knees, hips, and back. What you eat matters, too. Focusing on an anti-inflammatory diet rich in omega-3 fatty acids (think salmon and walnuts), antioxidants (berries and leafy greens), and lean proteins can help reduce joint inflammation from the inside out. Staying hydrated is also key, as water helps keep your cartilage lubricated. Simple swaps, like taking the stairs, stretching during your lunch break, and being mindful of your posture, all add up to create a more joint-friendly lifestyle and support your overall anti-aging goals.
Smart Exercise and Activity Choices
Many people worry that exercise will increase joint pain, but the right kind of movement is actually one of your best tools for protection. The goal is to strengthen the muscles that support your joints without overloading them. Low-impact activities like swimming, cycling, and walking are fantastic options. Incorporating weight-bearing and muscle-strengthening exercises helps improve joint function and can reduce pain by taking pressure off the cartilage itself. A physical therapist can be an incredible resource, helping you create a safe and effective routine tailored to your body. They can help you improve movement, build strength, and get you on the path to better joint regeneration.
Create Your Long-Term Maintenance Strategy
A proactive strategy is your best defense against joint degradation. It’s important to have realistic expectations: while non-surgical treatments can provide incredible symptom relief and improve your comfort, they don’t typically regrow lost cartilage. That’s why a consistent maintenance plan is so vital. The effectiveness of any approach, from physical therapy to regenerative medicine, can vary from person to person. The key is to find a personalized strategy that works for your body and lifestyle. Working with a specialist can help you build a comprehensive plan that combines lifestyle adjustments with advanced therapies, giving you a clear path forward. When you’re ready to build your plan, we’re here to help you get started.
Related Articles
- Cartilage Lesion Treatment & Regenerative Therapy | Miami Stem Cell
- Can Stem Cells Regrow Cartilage? Exploring Therapies – Stem Cell Therapy | Miami Stem Cell
- How to Avoid Knee Replacement for Bone on Bone Pain – Stem Cell Therapy | Miami Stem Cell
Frequently Asked Questions
How do I know if I need surgery or if regenerative medicine is a better fit? This is a great question, and the answer really depends on the extent of your cartilage damage and your personal goals. Surgery is often recommended for severe, extensive damage. However, for mild to moderate issues, regenerative medicine can be an incredibly effective way to manage pain and improve function without the long recovery. The best first step is a thorough evaluation with a specialist who can assess your specific situation and walk you through the pros and cons of each approach.
If cartilage doesn’t heal on its own, how do regenerative treatments actually work? You’re right, cartilage has a very poor ability to heal itself because it lacks blood flow. Regenerative treatments get around this problem by delivering a concentrated dose of your body’s own healing agents directly to the site of injury. Therapies using stem cells and exosomes don’t just mask the pain; they work on a cellular level to reduce inflammation and signal to your body’s tissues to begin the repair process, creating a healthier environment within the joint.
What is the recovery like for regenerative treatments compared to surgery? This is one of the biggest differences. Surgical procedures, like a joint replacement, often require weeks or even months of intensive rehabilitation and downtime. In contrast, regenerative treatments are minimally invasive procedures performed right in the office. Most people can return to their normal daily activities very quickly, with only minor restrictions on strenuous exercise for a short period. The goal is to get you back to your life with minimal disruption.
What’s the difference between PRP and stem cell therapy for joints? Think of it this way: Platelet-Rich Plasma (PRP) therapy uses a concentration of growth factors from your own blood to reduce inflammation and kickstart the healing process. It’s like sending in a specialized first-aid crew. Stem cell therapy is a more powerful approach that introduces new, versatile cells that can help regenerate tissue and orchestrate a more comprehensive repair. Which one is right for you depends on your specific condition, and a specialist can help determine the most effective option.
I’ve heard supplements like glucosamine can help. Are they enough to protect my cartilage? While some people find that supplements like glucosamine provide mild relief from joint discomfort, they don’t repair or regrow damaged cartilage. They can sometimes help with symptoms, but they don’t address the underlying structural problem. For true, long-term joint health, it’s important to focus on treatments that support your body’s ability to repair tissue and reduce the inflammation that causes damage in the first place.