Your body has a remarkable capacity to heal itself from cuts, broken bones, and other injuries. Yet, when it comes to joint cartilage, that natural ability seems to fall short, leaving millions to struggle with chronic pain and stiffness. This frustrating reality makes people wonder if there’s any way to kickstart that healing process. The central question becomes, can cartilage grow back if given the right signals and support? This is precisely the goal of stem cell therapy. It’s not about introducing a foreign substance, but about concentrating and directing your body’s own powerful repair cells to where they are needed most.
As more residents of Miami seek advanced treatments for joint issues, a common question arises: Can stem cells regrow cartilage? This query has gained attention due to stem cell therapy’s potential to revolutionize how we treat cartilage damage. At Stem Cell Miami, we’re dedicated to shedding light on how stem cell therapy for joint repair can offer new hope for those suffering from cartilage-related problems.
Understanding Cartilage and Its Challenges
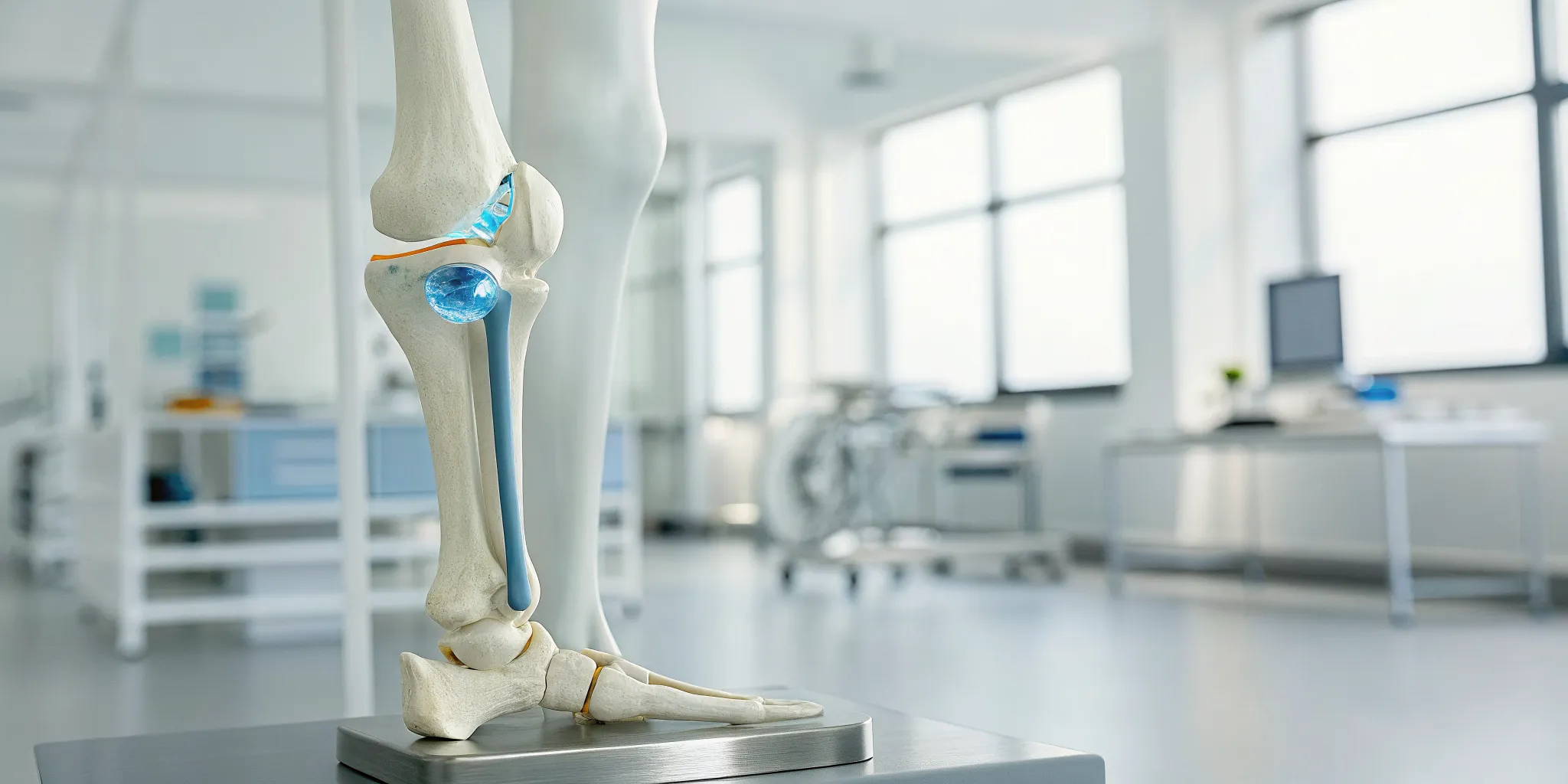
To appreciate the potential of regenerative medicine, it helps to first understand the unique nature of cartilage. Think of it as the smooth, protective cushion at the ends of your bones, allowing your joints to move freely and without friction. When this cushion gets damaged from an injury or deteriorates over time, it can lead to significant pain and stiffness. The central problem is that, unlike other tissues in your body, cartilage has a very limited ability to repair itself. This is why joint problems often become chronic, pushing people to search for solutions that go beyond temporary relief and address the underlying issue of tissue damage.
Why Cartilage Can’t Heal Itself
The main reason cartilage struggles to mend itself is its lack of blood supply. Most tissues in your body rely on blood vessels to deliver the oxygen, nutrients, and healing factors needed for repair, but cartilage doesn’t have this direct line. As researchers at Stanford Medicine point out, “Cartilage has almost no ability to heal itself once it’s damaged in adults.” This inherent limitation means that once cartilage is gone, it’s typically gone for good without intervention. This is why a knee injury from your twenties can still cause problems decades later and why conditions like osteoarthritis are progressive, making innovative treatments for joint regeneration so crucial for long-term health.
Hyaline vs. Fibrocartilage: The Difference Matters
When the body does attempt to repair cartilage damage, it often creates a patch with fibrocartilage—a type of scar tissue. While it’s better than nothing, fibrocartilage is structurally different from the original, smooth hyaline cartilage that lines your joints. It’s more fibrous and less durable, so it doesn’t provide the same smooth gliding motion and can break down more easily over time. The goal of advanced medical treatments isn’t just to fill a gap, but to encourage the growth of tissue that closely mimics the original hyaline cartilage. This distinction is key, as creating higher-quality tissue is essential for restoring true joint function and providing lasting relief from pain.
A New Perspective on Osteoarthritis
For a long time, osteoarthritis was simply seen as the result of “wear and tear”—an inevitable consequence of aging. However, scientists are now viewing it differently. According to a report in National Geographic, the modern view is that osteoarthritis is “a living biological process that can be influenced and potentially repaired.” This shift in perspective is a game-changer. It suggests that we don’t have to be passive bystanders to joint degeneration. Instead, we can use therapies that intervene in this biological process to slow down damage and actively promote healing, offering a more hopeful outlook for managing conditions like arthritis.
The Widespread Impact of Joint Problems
Joint pain isn’t a niche issue; it’s a widespread health concern that affects the daily lives of millions of people. From a dull ache that makes it hard to get out of bed to sharp pain that limits mobility, joint problems can significantly reduce a person’s quality of life. This isn’t just an issue for elite athletes or the elderly. People of all ages and backgrounds can experience joint damage due to injuries, genetic predispositions, or chronic conditions. The sheer number of individuals affected highlights the urgent need for effective, safe, and non-surgical treatment options that can provide meaningful and lasting relief.
Just How Common Is Joint Pain?
The statistics surrounding joint pain are staggering. According to data highlighted by Stanford Medicine, “Almost 1 out of every 4 adult Americans has arthritis.” That translates to over 55 million people dealing with the daily realities of this condition. This isn’t just a statistic; it represents millions of individual stories of canceled plans, frustrating physical limitations, and the ongoing search for effective pain management. When you consider the full spectrum of joint issues beyond arthritis, the number of people impacted is even larger. This widespread prevalence underscores why so many are turning to the field of regenerative medicine for new answers and lasting solutions.
What Is Stem Cell Therapy?
Stem cell therapy is a new treatment which leverages the body’s natural healing processes to repair damaged tissues. Stem cells possess a unique capacity to evolve into various cell types, including cartilage cells. This is crucial when discussing as it points to the potential of these cells to restore damaged cartilage caused by injury or aging.
How Does Stem Cell Therapy Work?
- Harvesting Stem Cells: The process begins with collecting stem cells from the patient’s own body, usually from bone marrow or fat tissue.
- Processing and Injection: The collected stem cells are processed and then injected into the affected joint.
- Regeneration Process: Once injected, these stem cells can transform into new cartilage cells, promoting the regeneration of damaged cartilage.
This approach directly addresses the question: Can stem cells regrow cartilage? It provides a promising answer for those dealing with joint pain and cartilage damage.
Advantages of Stem Cell Therapy for Joint Repair
Stem cell therapy offers several advantages for those seeking relief from joint issues:
- Reduced Inflammation: The therapy can help minimize inflammation in the affected joint.
- Enhanced Healing: Using the patient’s own cells lowers the risk of rejection and enhances healing.
- Pain Reduction: Many patients experience significant pain relief and improved joint function, which can significantly enhance their quality of life.
In Miami, stem cell therapy is becoming a sought-after option for addressing cartilage damage. By focusing on cartilage regeneration Miami, we at Stem Cell Miami aim to provide the community with effective treatment alternatives.
Comparing Surgical Options for Cartilage Repair
While regenerative medicine offers a promising, non-invasive path forward, it’s helpful to understand the surgical procedures traditionally used for cartilage repair. Knowing the full spectrum of options empowers you to make the most informed decision for your health. These surgical techniques have been the standard for years, but they each come with their own processes, recovery times, and potential outcomes. Understanding these methods can provide a clearer context for why many people are now exploring non-surgical approaches for joint regeneration and long-term relief.
Microfracture Surgery
Microfracture surgery is a technique where a surgeon creates tiny fractures in the bone underlying the damaged cartilage. The goal is to create a controlled injury that stimulates a healing response, allowing new, cartilage-like tissue to form. This procedure is typically reserved for smaller areas of cartilage damage. While it can provide relief, the new tissue that grows is fibrocartilage, which is more like a scar tissue than the smooth, durable hyaline cartilage that originally lined the joint. Because of this, the results can be less predictable long-term, often making it a temporary solution for many patients seeking lasting pain management.
Matrix-Induced Autologous Chondrocyte Implantation (MACI)
MACI is a more complex, two-step procedure designed to regrow healthy cartilage. In the first surgery, a small sample of your own healthy cartilage cells (chondrocytes) is harvested from a non-weight-bearing area of your knee. These cells are then sent to a lab to be multiplied over several weeks. In a second surgery, the newly grown cells are implanted back into the damaged area on a special collagen patch, where they can mature into new tissue. While MACI has shown to be effective for treating specific types of cartilage damage, it requires two separate invasive procedures and a significant recovery period, which is a major consideration for many individuals.
Osteochondral Autograft and Allograft Transplantation (OATS)
The OATS procedure, sometimes called mosaicplasty, involves transferring healthy cartilage along with the underlying bone to the damaged area. Think of it like moving a small plug of healthy lawn to a bare patch. If the tissue comes from your own body (autograft), it’s taken from a non-weight-bearing part of the same joint. If a donor’s tissue is used (allograft), it’s carefully screened and prepared. This technique is often used for active individuals because it replaces the damaged area with mature, functional cartilage. However, the autograft approach creates a new injury site where the plug was taken, and the availability of donor tissue for allografts can be limited.
What to Expect from Stem Cell Therapy
Expectations for joint repair stem cell therapy:
- Initial Consultation: You will meet with our staff to discuss your issue and treatment choices.
- The Procedure: Stem cell injection is minimally invasive and typically performed on an outpatient basis.
- Recovery Period: To aid recovery after the procedure, you will need to follow specific guidelines, such as engaging in physical therapy and avoiding strenuous activities.
Who Is a Good Candidate for Cartilage Repair?
Determining if you’re a good candidate for cartilage repair is a crucial first step. Traditionally, the ideal person for these procedures is often younger, typically under 50, with a specific, isolated area of cartilage damage rather than widespread arthritis. However, regenerative medicine is changing that conversation. Treatments like stem cell therapy can be effective for a broader range of individuals dealing with joint degeneration. The key is a thorough evaluation. A personalized consultation allows a specialist to assess the extent of your cartilage damage, discuss your health history, and determine if a regenerative approach can help you achieve your goals for pain relief and improved mobility. This ensures you receive a treatment plan tailored specifically to your condition and needs for joint regeneration.
The Importance of Post-Treatment Care and Physical Therapy
The success of any cartilage repair treatment doesn’t end when you leave the clinic. Your commitment to post-treatment care is just as important as the procedure itself. Following your therapy, a structured physical therapy program is essential for a full recovery. This isn’t just about rebuilding strength; it’s about guiding the new tissue to grow correctly and ensuring your joint regains its stability and function. Your care plan will likely include specific exercises to improve range of motion, along with guidelines on activities to avoid as you heal. Think of it as a partnership with your body—the stem cell therapy provides the building blocks for repair, while your dedication to physical therapy provides the framework for a strong and lasting recovery.
Can Supplements or Diet Regrow Cartilage?
Many people wonder if they can simply eat certain foods or take supplements to regrow damaged cartilage. While a healthy diet rich in anti-inflammatory foods is excellent for overall joint health, there is no scientific evidence that diet or supplements can rebuild lost cartilage. Products containing glucosamine and chondroitin may offer some relief from joint pain and swelling for certain individuals, but they don’t address the underlying structural damage. They manage symptoms, but they don’t fix the root cause. This is where regenerative treatments differ. Instead of just masking the problem, therapies like those offered at Miami Stem Cell are designed to work with your body’s natural healing mechanisms to repair the tissue itself, offering a more direct solution.
The Future of Cartilage Regeneration
As research advances, the potential for stem cells to regenerate cartilage and address joint issues continues to grow. Innovations in stem cell technology are likely to enhance the effectiveness of treatments, offering greater hope for individuals suffering from cartilage degeneration and joint pain.
Harnessing the Body’s “Salamander-like” Repair Mechanisms
For a long time, the prevailing belief was that once your cartilage was gone, it was gone for good. However, groundbreaking research is changing that perspective. Scientists have discovered that human joints possess a “salamander-like” ability to repair their own cartilage, challenging everything we thought we knew. This research, highlighted by Duke Health, suggests our bodies have innate, powerful mechanisms for self-repair, similar to how some animals regrow entire limbs. This finding is the cornerstone of regenerative medicine. Instead of just managing symptoms, the goal is to work with your body’s natural healing potential. At Miami Stem Cell, our approach to joint regeneration is built on this very principle: amplifying your body’s inherent ability to heal and restore damaged tissue from within.
Emerging Treatments: From Chemical Signals to Gene Therapy
Building on the discovery of our body’s repair capabilities, researchers are now exploring ways to guide and enhance this process. For instance, a team at Stanford Medicine developed a method that uses specific chemical signals to direct the body’s own stem cells to the site of an injury, encouraging them to form new, healthy cartilage. Other scientists are tackling the problem from a different angle. As reported by National Geographic, researchers are using gene therapy to halt the inflammation that rapidly destroys cartilage in conditions like arthritis. These innovative strategies represent the next frontier in joint health, moving beyond simple repairs to sophisticated, targeted biological solutions that address the root cause of cartilage damage.
A Note on Treatments in Development
While many of these cutting-edge techniques, like gene therapy, are still in the research and development phase, they signal a major shift in how we approach joint care. The science behind them validates the core concepts of regenerative medicine that are available today. The treatments we utilize at Miami Stem Cell are grounded in this same forward-thinking science, using the body’s own powerful healing agents to promote repair. We are committed to providing therapies that are not only innovative but also adhere to strict safety and regulatory standards, offering a reliable alternative to treatments you might find elsewhere. You can learn more about the importance of these standards by understanding the difference between overseas vs. USA stem cell treatments.
Conclusion
The question of Can stem cells regrow cartilage is more than a theoretical concern; it’s a practical consideration for those exploring advanced treatment options. At Stem Cell Miami, we’re committed to offering cutting-edge solutions in cartilage regeneration and stem cell therapy for joint repair. If you’re dealing with cartilage issues and are curious about how stem cell therapy might help, we invite you to reach out to us for a consultation.
Frequently Asked Questions
How is stem cell therapy different from surgical options like microfracture? Surgical procedures like microfracture work by creating a controlled injury to stimulate a healing response. However, this often results in the growth of fibrocartilage, which is more like a scar tissue and isn’t as durable as your original joint lining. Stem cell therapy takes a different approach. It introduces a high concentration of your body’s own repair cells to the area, encouraging the growth of tissue that more closely resembles the smooth, resilient hyaline cartilage needed for proper joint function, all without an invasive surgical procedure.
How long does it take to feel a difference after the treatment? This isn’t an overnight fix; your body needs time to do its work. While some people notice a decrease in inflammation and pain within a few weeks, the real magic happens over several months as the stem cells signal repair and new tissue begins to form. The timeline is unique to each person and depends on the extent of the joint damage and your body’s individual healing response.
Is this a permanent solution for my joint pain? The goal of stem cell therapy is to repair the underlying tissue damage, which can provide significant and long-lasting relief that you wouldn’t get from treatments that only mask symptoms. For many people, this can be a long-term solution that helps them avoid or delay surgery for years. However, the longevity of the results can be influenced by your lifestyle, the severity of your condition, and the natural aging process.
I have advanced osteoarthritis. Am I still a candidate for this therapy? While it’s true that treating a single, isolated injury can be more straightforward, stem cell therapy can still be highly effective for individuals with more widespread osteoarthritis. The therapy works to reduce the chronic inflammation that drives arthritic pain and can help improve overall joint function. Even if it doesn’t completely reverse every aspect of arthritis, it can significantly improve your quality of life and mobility. A personal consultation is the best way to determine if it’s the right fit for you.
What makes the stem cells used at your clinic different from those used in other countries? This is a crucial question, and it comes down to safety and regulation. At Miami Stem Cell, we adhere to the strict guidelines set by the FDA. We use umbilical cord-derived mesenchymal stem cells that are sourced from reputable tissue banks and processed in a controlled, sterile environment. This ensures you receive a safe, high-quality product. Many clinics overseas operate with far less oversight, which can introduce risks related to the quality and viability of the cells, making it essential to choose a provider you can trust.
Key Takeaways
- Target the root cause of joint pain: Stem cell therapy works with your body’s natural healing mechanisms to repair damaged cartilage directly, offering a more fundamental solution than treatments that only manage symptoms.
- Explore non-surgical options first: Before considering invasive surgery, understand that regenerative medicine provides a minimally invasive alternative for joint repair, helping you avoid the significant downtime and recovery associated with traditional procedures.
- Your recovery is an active process: A successful outcome is a partnership. The best results combine the regenerative procedure with your commitment to post-treatment care, especially a personalized physical therapy plan designed to restore strength and function.
Related Articles
- 5 Best Treatments for Cartilage Protection
- Can Stem Cells Regrow Cartilage? Exploring Therapies
- Revolutionizing Joint Health: Can Stem Cells Regrow Cartilage?
- Cartilage Lesion Treatment & Regenerative Therapy